How prevalent is recovery from opioid use disorder in the United States and how do people get there?
The sharp increase in opioid use related harms highlights how little is known about opioid use disorder recovery. This study examined data from a nationally representative sample of U.S. adults who once had an opioid problem to document patterns of recovery from opioid misuse, as well as factors related to early (<1 year) and mid-recovery (1-5 years) status. Findings help inform policy, prevention, and practice recommendations.
WHAT PROBLEM DOES THIS STUDY ADDRESS?
The rising incidence of opioid misuse in recent decades has resulted in an unprecedented increase in opioid use disorder, opioid use-related injury, and economic burden. In addition, rates of opioid overdose death have increased from below 10,000 in 1999 to 47,600 in 2017 and 46,802 in 2018. Efforts to understand, prevent, and reduce the rising incidence of opioid use at the population level (e.g., reducing overdose within states and counties) over the past few years have been promising, yet remarkably little is known about factors associated with recovery of opioid misuse at the individual level which, if known, could improve policies, treatment, and recovery support services.
In this large-scale and nationally-representative survey of U.S. adults who resolved a significant substance use problem, the authors examine the prevalence of early recovery (<1 year since problem resolution), and mid-recovery (1-5 years since problem resolution) status, and provide a first look at the characteristics of individuals who have achieved early vs. mid-recovery from opioids and compare this group to those achieving recovery from alcohol use problems. The authors also provide insight into effective patterns of service utilization, as well as implications for policy, outreach, and intervention to promote long-term recovery.
HOW WAS THIS STUDY CONDUCTED?
This study was a secondary analysis of a nationally representative survey of U.S. adults who resolved a significant substance use problem, called the National Recovery Study. In the current analysis, authors focused specifically on participants who identified opioids as their primary substance and compared these individuals to those who identified alcohol as their primary substance on demographic characteristics, substance use history, service utilization, and markers of psychosocial wellbeing. Individuals were randomly selected from 97% of listed households in the U.S. and benchmarked using demographics in proportion to the known U.S. population.
Of the 39,809 individuals contacted, 25,229 (63.4%) completed the eligibility screening item. The final sample used in the current analysis included 2,002 respondents who answered “yes” to “Did you used to have a problem with drugs or alcohol, but no longer do?” The researchers then used procedures to assign differential “weights” to participants to ensure proportional representation among the study sample relative to the known U.S. population (i.e., to accurately reflect proportions of individuals across sex, age, race/ethnicity, geography, education, income, metropolitan area, and home ownership). Gathering data in this way, coupled with the authors’ use of demographic weighting strategies, allowed them to provide population-based estimates of the rate of resolving a primary opioid vs. alcohol problem, and information about the characteristics of individuals who have achieved recovery nationwide.
Study authors provided population-based estimates of the prevalence of recovery from opioid and alcohol misuse in the U.S. population, by measuring substances participants used more than 10 times in their lifetime, which of these substances were ever a “problem” for them, which of these “problem” substances was their primary “substance of choice.” Participants also answered questions about their history of participating in formal treatment (e.g., detoxification, residential or outpatient treatment), mutual-help groups (e.g., Alcoholics Anonymous [AA], Narcotics Anonymous [NA]), recovery support services (e.g., sober living housing), and use of medications approved for opioid use disorder (e.g., acamprosate, disulfiram, naltrexone). Lastly, participants answered questions about overall psychological distress, happiness, and self-esteem.
The researchers then examined differences between participants with less than 1 year of recovery (“early recovery”) from opioids vs. alcohol, then 1-5 years of recovery (“mid-recovery”) from opioid vs. alcohol, on measures of treatment received, mutual-help group attendance, medications used, and psychological well-being variables measured.
WHAT DID THIS STUDY FIND?
A total of 5% reported opioids and 51% reported alcohol as their primary substance, corresponding to population estimates of nearly 1.2 million and 11.4 million in the U.S. who have resolved opioid and alcohol use problems, respectively.
Notably, just over 1% (population estimate: 259,260) vs. 7% (population estimate: approx. 1.6 million) resolved opioid vs. alcohol use problems in the past year; just over 2% (estimated 489,465) vs. 12% (estimated 2.6 million) resolved their opioid vs. alcohol use problems in the last 1-5 years.
Compared to individuals in early recovery from alcohol (<1 year), individuals in early recovery from opioids were younger (27.5 vs. 39.6 years old), more likely to be White (94.3% vs. 61.4%), began using their primary substance later in life (18.3 vs. 15.1 years old), and reported use of more substances overall.
Individuals with primary opioid use also used for an average of 8.4 years before resolving their problem, compared to 21.9 years among those reporting primary alcohol use.
Individuals in mid-recovery (achieved 1-5 years of opioid recovery) also reported use of more “problem” substances previously, used opioids for an average of 9 years (compared to 23 years for primary alcohol users), and were older when they first started using opioids (22.4 vs. 15.3 years for primary alcohol users).
Individuals in early recovery evidenced similar patterns of treatment, mutual-help, recovery support, and medication use, but individuals in mid-recovery from opioids reported significantly greater utilization of each compared to individuals in mid-recovery from alcohol use (see Figure 1).
Individuals in mid-recovery from opioids were more likely to report use of medication to treat substance use disorder (e.g., buprenorphine) and attended more Narcotics Anonymous (NA) meetings.
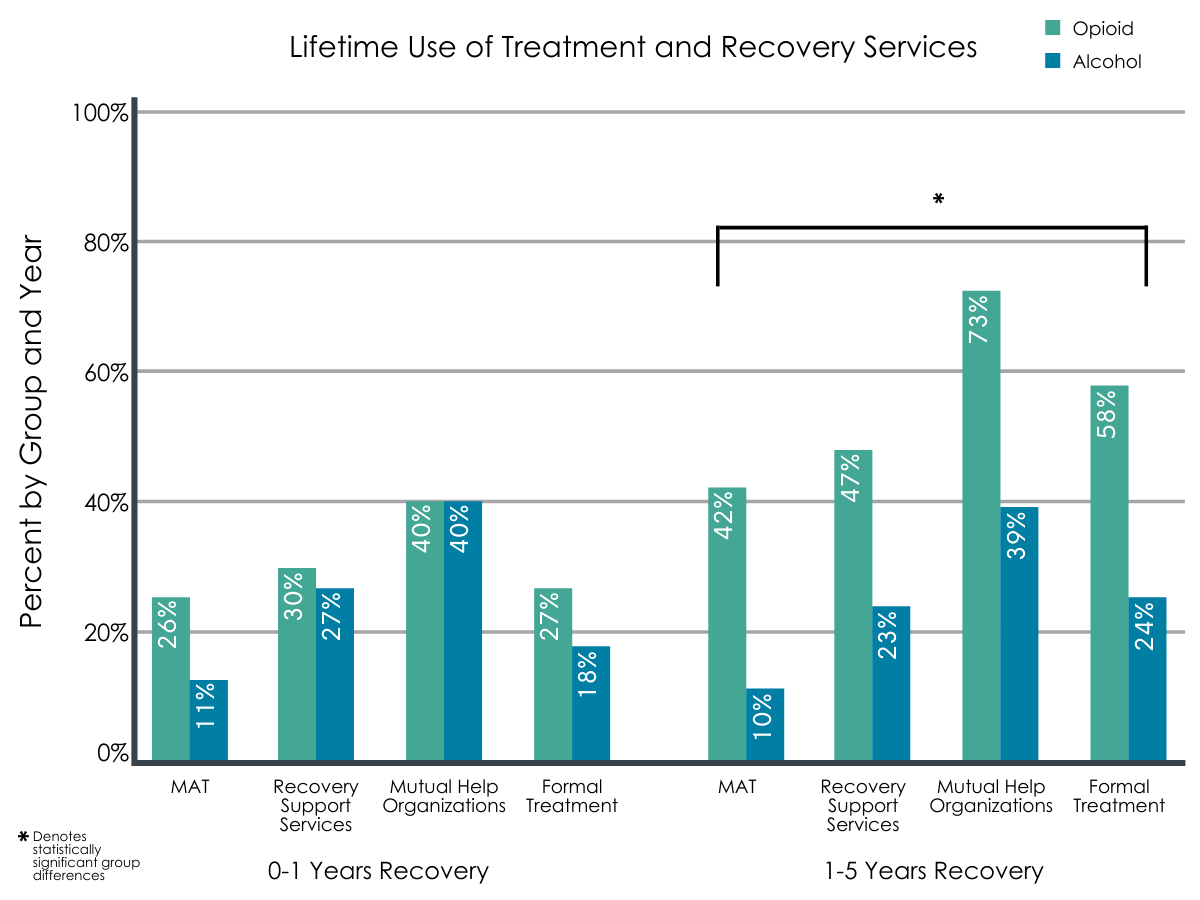
Figure 1.
Lastly, self-esteem scores were higher among individuals in early recovery from opioids compared to those in early recovery from alcohol, but the opposite was true for individuals in mid-recovery (Figure 2). Opioid and alcohol primary participants in both early and mid-recovery had similar levels of other psychological and social well-being (e.g., current psychiatric symptoms).
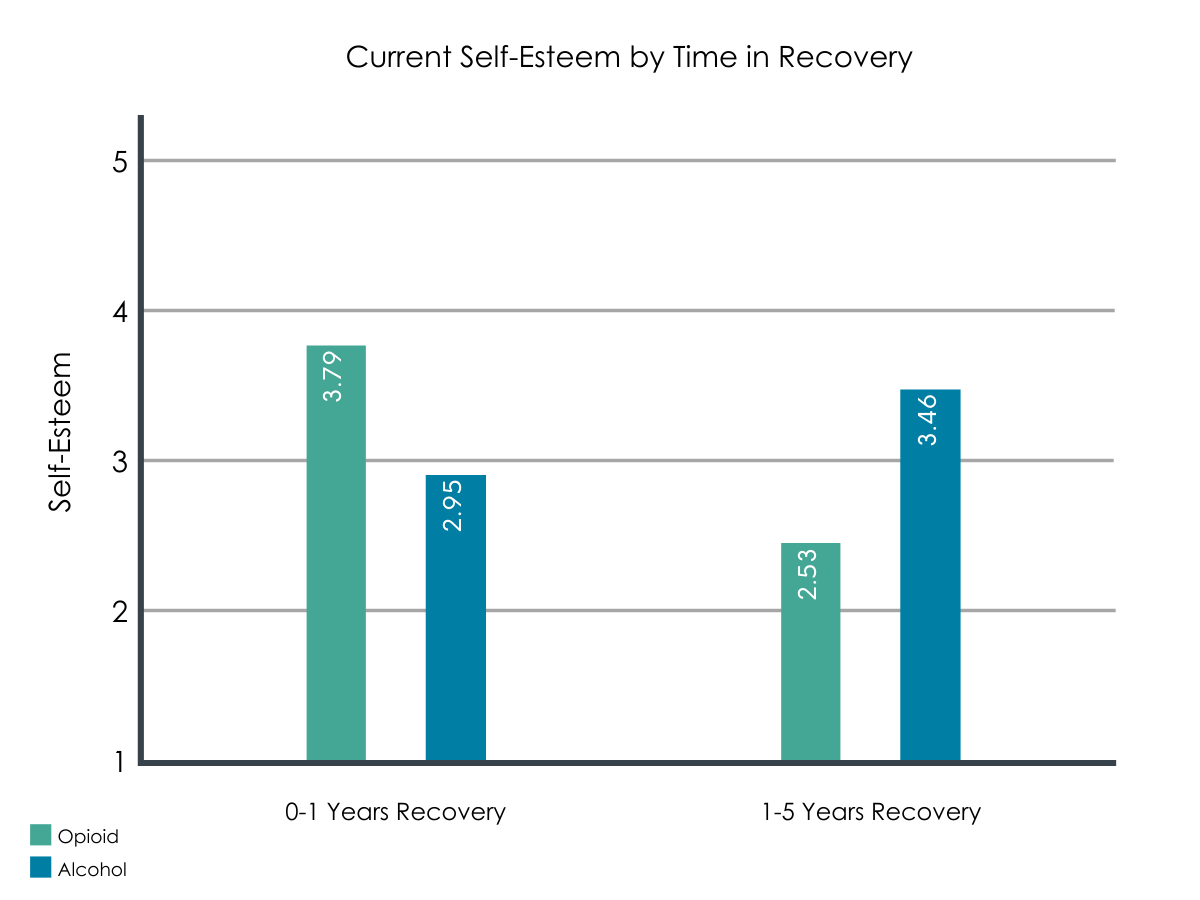
Figure 2.
WHAT ARE THE IMPLICATIONS OF THE STUDY FINDINGS?
This study provides the first known estimates of opioid and alcohol use recovery, as well as information into key demographic and service utilization variables associated with recovery. Nearly 1.2% (estimated 259,260) and 2.2% (estimated 489,465) of primary opioid users achieved recovery for up to a year or 1-5 years, respectively. Though encouraging, these results should be interpreted in light of estimates that 10.6 million in the U.S. report past-year opioid misuse, nearly 2 million have opioid use disorder, and persistently high rates of opioid overdose and death. This disparity highlights existing service gaps with respect to the ongoing opioid epidemic, as well as the potential good that would likely result from dissemination of policy, outreach, and prevention and intervention improvements.
Although the proportions of individuals in recovery were higher for individuals with primary alcohol use (estimated 1.6 million in early recovery, 2.6 million in mid-recovery), it should be noted that the public health, personal, and economic costs of alcohol continue to outweigh those of opioids and, therefore, also require ongoing attention in terms of policy, research, and intervention.
Compared to individuals in early alcohol recovery, those in early recovery from opioids were younger, more likely to be White, reported more extensive substance use in the past, and began using opioids at an older age. Similarly, among those in mid-recovery, individuals with primary opioid use reported use of more substances previously and began using their primary drug (opioids) later in life. In both recovery groups, individuals reporting primary opioid use used for an average of 8-9 vs. 22-23 years for primary alcohol users. By considering the unique needs of individuals in, or seeking, opioid use disorder recovery, treatment providers and policy makers may help address their greater complexity and psychosocial needs.
Treatment service and mutual-help utilization rates were similar among opioid and alcohol groups in early recovery. However, rates of treatment utilization, service use (e.g., sober living housing), mutual-help group attendance, and medication use were significantly higher among primary opioid users compared to primary alcohol users in mid-recovery. This may signify need for greater breadth, intensity and/or duration of treatment for opioid users, as well as ongoing use of medications to manage symptoms and cravings, to achieve recovery past 1 year. This may be due in part to prior findings which show those with primary opioid problems have substantially lower recovery resources (“recovery capital”) and much lower quality of life and functioning in the early years of recovery compared to individuals with other alcohol or drug use problems. As such those with primary opioid problems may need ongoing and more intensive support for longer periods than other groups.
In addition, medications for opioid use disorder (e.g., buprenorphine, methadone) receive relatively more attention within medical and scientific communities, with lower rates of use and adoption of these evidence-based treatments in the real world. Greater attention and outreach may help offset negative attitudes toward medications for opioid use disorder to promote patient access and adoption of these evidence-based treatments.
- LIMITATIONS
-
- The cross-sectional nature of this study and reliance on single-item self-report measures limits directional and causal inference, as well as an inability to distinguish between self-rated and diagnostic thresholds for substance use disorder and recovery from opioid and alcohol use.
- The authors measured opioid use/recovery broadly and were unable to differentiate between different types of opioid use (e.g., heroin vs. misuse of prescription medication).
- The sampling strategy used either limited or did not allow for recruitment of participants who are homeless or currently in inpatient or residential treatment settings, sober living houses, or who are incarcerated.
- The authors were unable to compare characteristics of individuals who achieved recovery to those who had not.
- The authors limited groups based on recovery in relation to their primary substance of choice. This may have overlooked forms of polysubstance use, or subsequent use of other substances, like alcohol, among participants with remitted opioid use problems. It is possible that individuals who reported opioid use recovery later began using other substances, like alcohol, which could account for the lower levels of self-esteem among those in mid-recovery from opioids. Finally, it is also possible that they reported recovery from their primary substance but did not consider opioids their “primary” substance. This could have resulted in misclassification to the extent that participants recovered from one primary substance but not opioids.
BOTTOM LINE
- For individuals and families seeking recovery: The results of this study suggest that many U.S. adults have resolved opioid and alcohol problems. Compared to individuals for whom alcohol was their primary substance, those in early recovery from opioids were younger, used more substances, started using their opioids at an older age, and were more likely to be White. Time to cessation following initiation was between 8-9 years for opioids and 22-23 years for alcohol. This could be due to the nature of opioid use and opioid users incurring negative consequences more quickly (e.g., health, legal), hastening treatment seeking and benefit. Individuals and families should remain aware that the progression of opioid use initiation to disorder is typically more rapid than that of alcohol, nicotine, cannabis, and cocaine, making early detection and intervention critical given it is more lethal. Lastly, results of this study support the use of formal treatment, recovery support services (e.g., sober living houses), mutual-help groups (e.g., AA, NA), and medications for addiction treatment (e.g., buprenorphine, naloxone). This was evidenced by higher rates of utilization of each among individuals with 1-5 years of opioid recovery.
- For treatment professionals and treatment systems: These results highlight rates of successful recovery among individuals reporting past problems with opioids and alcohol. In particular, and relative to individuals with primary alcohol use, those in mid-recovery from opioid use reported greater service utilization, mutual-help group attendance, and medication use. The fact that being younger and White differentiated individuals with early opioid vs. alcohol recovery, yet these demographics did not differentiate between mid-recovery groups, suggests that individuals who are younger and/or White might be at greater risk of relapse after the first year. Clinicians should be mindful of this possibility and systems should take into account that individuals with between 1 and 5 years of opioid recovery benefited from an array of services prior to achieving recovery.
- For scientists: This is the first known U.S. population-based survey of opioid use recovery to date. The results of this study suggest promising rates of recovery among individuals with primary opioid and alcohol use. Factors associated with early opioid recovery, relative to early alcohol recovery, included young age, White race, greater number of past substances used, older age of primary opioid use onset and shorter duration of use prior to cessation. Being younger and White differentiated individuals with early opioid vs. alcohol recovery but not mid-recovery groups. Lastly, rates of service utilization, mutual-help group attendance, and medication use were greatest among individuals in mid-recovery from opioids, suggesting perhaps greater necessity of intervention breadth, intensity, and duration to achieve recovery past 1 year. These novel and important findings would benefit from replication. Future research would benefit from diagnostic assessment of substance use disorder and recovery; collection of information from individuals who have not achieved recovery; and enhanced measurement to differentiate types of opioid use/patterns of use, monitor substance use changes over time, and track use of secondary and tertiary substances (e.g., alcohol use among primary opioid users). Future research could also examine what combinations of services are most helpful.
- For policy makers: Individuals in recovery from opioid use problems and disorder access a variety of services that include, but are not limited to, behavioral interventions (e.g., residential and outpatient treatment), medication (e.g., buprenorphine, methadone, naltrexone), recovery support services (e.g., sober living houses, state/local community organizations), and mutual-help groups (e.g., AA, NA). At the same time, additional policy and outreach are needed to reduce risk of overdose death, and promote conversion from opioid disorder to recovery. Further implications of this study are that early detection and intervention are key for opioid use, given the shorter duration between initiation and disorder, and that individuals who are younger and/or White might be less likely to sustain recovery past 1 year. At the same time, ongoing funding for opioid use disorder research can help provide information regarding best practices and policies to maximize recovery and quality of life outcomes for these at-risk individuals.
CITATIONS
Hoffman, L. A., Vilsaint, C., & Kelly, J. F. (2019). Recovery from opioid problems in the US population: Prevalence, pathways, and psychological well-being. Journal of Addiction Medicine, [Epub ahead of print]. doi: 10.1097/ADM.0000000000000561

