Do Body Responses to Reward & Stress Indicate Time in Recovery from Opioid Use Disorder?
Opioid use disorders are characterized by disruptions in several areas of functioning, including neurobiological (e.g., impaired reward circuitry) and physiological (e.g., increased baseline levels of stress) domains. Consequently, it stands to reason that improvements in these domains could serve as biological markers of recovery as well.
Indeed, some data suggest that biologically-mediated measures of reduced sensitivity to natural rewards (e.g., socializing with friends) predict relapse in recovering opioid addicts. Generally, however, the field knows relatively little about how stress and reward-related biological markers change as the recovering individual accrues abstinence.
Moreover, pharmaceutical opioid misuse and use disorders have increased dramatically during the last 15 years, though heroin addiction has received more attention in the addiction and recovery literature to date.
Bunce et al. used cross-sectional methodology to begin to address these gaps in the science by comparing three groups of patients with DSM-IV pharmaceutical opioid dependence, recruited from a residential treatment program in Pennsylvania: recently detoxified individuals (n = 7); individuals attending residential treatment for 2-3 months (n = 7); and healthy controls (made up of program staff with no history of addiction) (n = 7). The average participant was between 33-40 years old, female, and had at least some college. Seven had a current mood disorder and 10 a current anxiety disorder.
Those receiving medication assisted treatment (agonist, e.g., suboxone, and antagonist, e.g., naltrexone) or with past-year dependence on a non-opioid drug, including alcohol, were excluded. Brain activity was measured by hemoglobin concentrations via fNIR (function near-infrared spectroscopy) in response to pictures of opioid pills and natural rewards (e.g., food), and stress was measured by cortisol levels during the day and evening as well as sleep patterns.
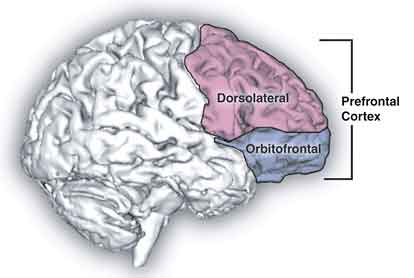
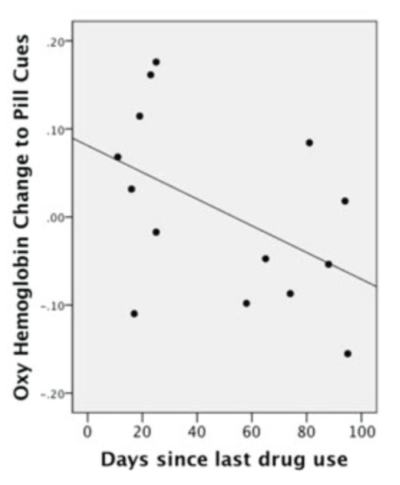
There was a moderate recovery-reactivity relationship for both sets of cues such that greater time in recovery predicted less brain reactivity.
Similarly, recently detoxified patients showed the highest levels of daytime and evening cortisol, as well as disrupted sleep, while residential treatment and healthy controls were not different. Again, recovery time was positively correlated with lower cortisol and increased sleep (better outcomes).
IN CONTEXT
This interesting multidisciplinary study serves as part of a unique, budding literature examining biophysiological markers of substance use disorder recovery.
The data suggests that recently detoxified patients devote greater attentional resources when presented with drugs, and with increased recovery time, this attentional bias may be reduced. Authors suggest that the residential treatment group may devote even fewer attentional resources than healthy controls due to treatment-based conditioning to manage drug-related cues.
- LIMITATIONS
-
Beyond the study’s small sample (which is common in complex, expensive investigations of brain and physiological functioning), we encourage the reader to be mindful of the cross sectional nature of the study, as change over time was not observed in the same group of individuals over time, so factors other than time in recovery could explain the differences between groups. Also, the group of healthy controls – staff at a residential treatment facility – was used for convenience of data collection but, given their ongoing indirect exposure to patients’ addiction and recovery experiences, it is uncertain whether they are an optimal representation of “normal” brain/reward and stress reactivity.
BOTTOM LINE
- For individuals & families seeking recovery: This study indicates that throughout recovery progression, it is likely to notice improvements in many areas of functioning including lowered reactivity to drug cues, increased reactivity to real-world rewards, and improved sleep.
- For scientists: Although limited by its small sample size, cross-sectional methodology, and convenience group of healthy controls, this study represents a sound approach on which to build additional longitudinal investigations of biophysiological markers of recovery and relapse risk.
- For policy makers: The long-term vision of recovery research should take into account not only treatment and recovery-related behavioral outcomes (abstinence) but also biophysiological markers that contribute to a more comprehensive model of relapse and recovery.
- For treatment professionals and treatment systems: Although much work may be needed early on to help patients manage functioning related specifically to their SUD and the ways it disrupted their lives, these preliminary data suggest cue-reactivity and self care is likely to improve with time allowing for greater opportunity to address more complex issues (e.g., relationships, employment/educational/career advancement, etc.)
CITATIONS
Bunce, S. C., Harris, J. D., Bixler, E. O., Taylor, M., Muelly, E., Deneke, E., … & Meyer, R. E. (2015). Possible evidence for re-regulation of HPA axis and brain reward systems over time in treatment in prescription opioid-dependent patients. Journal of addiction medicine, 9(1), 53-60.

