What’s Driving America’s Overdose Crisis?
More people are dying each year from overdose than died during the peak of the AIDS epidemic. This article explores the factors driving this crisis and indicates critical steps to address this situation.
WHAT PROBLEM DOES THIS STUDY ADDRESS?
The US is currently experiencing an unprecedented health crisis. Drug overdose was responsible for 52,404 deaths in 2015, and provisional data from the US Centers for Disease Control and Prevention (CDC) indicate drug overdose deaths increased again by more than 20% in 2016 to 64,070. Experts believe the situation worsened further through 2017. It is critical that we understand the factors driving these overdose deaths and the opioid overdose crisis, which makes up the majority of these deaths, so we can develop better, evidence-based solutions to address this unprecedented health emergency.
HOW WAS THIS STUDY CONDUCTED?
This opinion piece published in the Journal of the American Medical Association (JAMA) summarizes epidemiological data collected by the Centers for Disease Control and Prevention (CDC), Substance Abuse and Mental Health Services Administration (SAMHSA), and Drug Enforcement Administration (DEA), on the current overdose death crisis in the US. The authors also speculate on factors driving the massive increase in overdose deaths in recent years, and suggest actions to remedy this dire situation.
WHAT DID THIS STUDY FIND?
The authors summarize data from the CDC indicating drug overdose accounted for 52,404 deaths in the United States in 2015. Provisional data suggest drug overdose deaths increased again from 2015 to 2016 by more than 20% (from 52,898 deaths in the year ending in January 2016 to 64,070 deaths in the year ending in January 2017). Increases were greatest for overdoses related to opioids, including illicitly manufactured fentanyl, which more than doubled, accounting for more than 20,000 overdose deaths in 2016, compared to 10,000 deaths in 2015. This difference is enough to account for nearly the entire increase in drug overdose deaths from 2015 to 2016.
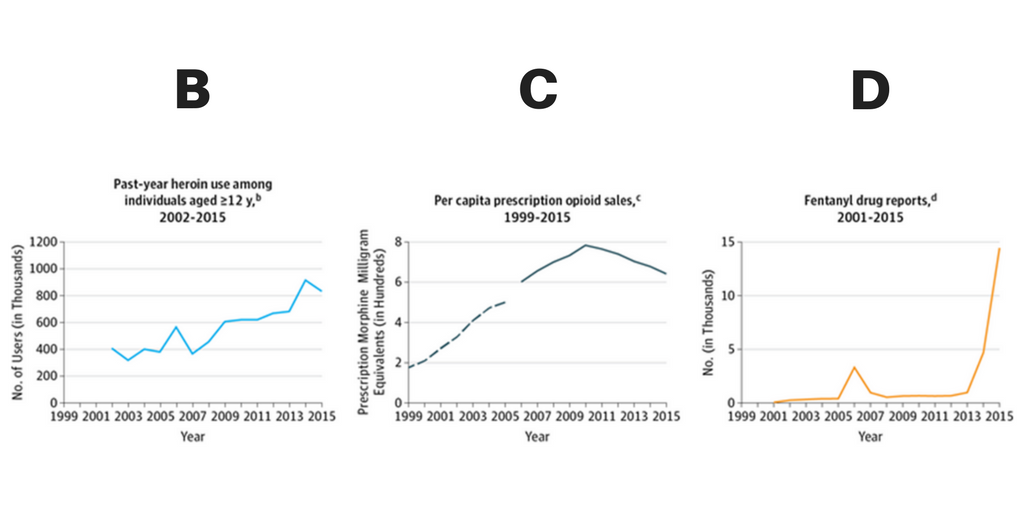
Dowell and colleagues note too that since 2010, overdose deaths involving predominantly illicit opioids (heroin, synthetic non-methadone opioids, or both) have increased by more than 200% (Figure A). The dramatic increase in opioid-related overdose deaths appears to have little to do with changing trends in heroin use. Data from the National Survey on Drug Use and Health and DEA reveal only moderate increases in people reporting past-year heroin use from 2010 to 2015 (Figure B), and decreases in the prescription of opioids (Figure C). The authors propose that the dramatic increase in opioid-related deaths is largely being driven by the increased availability of fentanyl, a synthetic opioid approximately 50 times more potent than heroin.
What are the next steps to bring this situation under control?
- First, reduce unnecessary exposure to prescription opioids to prevent opioid use disorder. Despite recent progress, 3 times the amount of opioids were prescribed in 2015 compared with 1999. Among people ultimately entering treatment for opioid use disorder, the proportion starting with prescription opioids rather than heroin has decreased from more than 90% in 2005 to 67% in 2015. However, prescription opioid exposure remains a clear path to opioid addiction.
- Opioid use disorder treatment should become a routine part of medical care, with expectations that all practices have adequate capacity to provide effective treatment. Treatment should be available for patients with opioid use disorder and at risk for overdose, starting with those who survive a drug overdose.
- Emergency department protocols could be developed to provide buprenorphine (Suboxone) induction and short-duration buprenorphine prescriptions to bridge individuals with opioid use disorder coming to the ED to longer-term treatment.
- Greater collaboration with law enforcement is necessary to link preventive services and effective treatment. For example, providing medications to support opioid addiction recovery in prisons increases the probability that incarcerated persons with opioid use disorder, who are at high risk of overdose after release, will engage with treatment after release.
- First responders and close associates of people who use drugs need adequate supplies of naloxone and training to reverse opioid overdose, so those who overdose can be kept alive and have a chance to start treatment.
- Collection of real-time data are needed to drive rapid, coordinated community responses to increases in opioid overdoses. The CDC is working with 32 states and the District of Columbia to improve use of syndromic surveillance and emergency medical services data and identify increases in overdoses more quickly.
- Educate patients and communities about the risks of opioids. People with opioid use disorder and their families need to know about effective treatments, so that resources and lives are not squandered pursuing ineffective or harmful therapies. People who use drugs require education about the risks of fentanyl contamination in heroin and other drugs, including cocaine and counterfeit prescription opioids. In most areas of the United States people who use heroin should assume the local supply is contaminated with fentanyl.
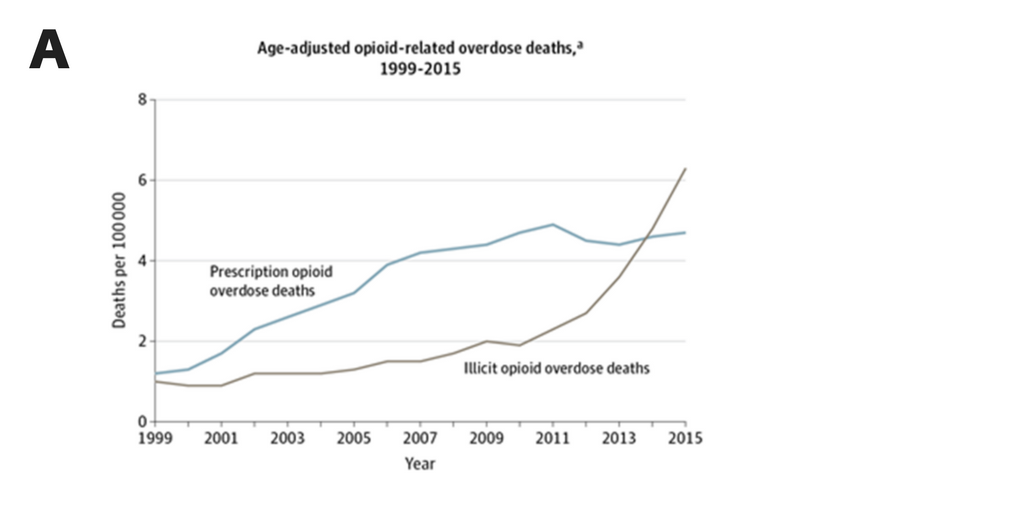
A Source: National Center for Health Statistics at the US Centers for Disease Control and Prevention. WONDER online database: prescription opioid overdose deaths include fatal overdoses related to natural and semisynthetic opioids or methadone. Illicit opioid-related overdose deaths are related to heroin or synthetic nonmethadone opioids, and some overdose deaths are related to prescribed fentanyl or other prescribed synthetic opioids.
B Source: Substance Abuse and Mental Health Services Administration. National Survey on Drug Use and Health. https://www.samhsa.gov/data/population-data-nsduh/reports?tab=38.
C Sources: Dashed line from 1999 to 2005 (Drug Enforcement Administration. Automation of Reports and Consolidated Orders System: sales to pharmacies, hospitals, and practitioners for codeine, fentanyl, hydrocodone, hydromorphone, meperidine, methadone, morphine, and oxycodone. Paulozzi LJ, et al. MMWR Morb Mortal Wkly Rep. 2011;60:1487-1492). Solid line from 2006 to 2015 (QuintilesIMS estimates of opioid prescriptions dispensed in the United States to 59 000 pharmacies, representing 88% of US prescriptions. Guy GP Jr, et al. MMWR Morb Mortal Wkly Rep. 2017;66:697-704).
D Source: Drug Enforcement Administration. Fentanyl, 2001-2015. https://www.deadiversion.usdoj.gov/nflis/2017fentanyl.pdf. The number of fentanyl drug reports reflects the number of encounters by law enforcement that tested positive for fentanyl. Therefore, fentanyl drug reports provide an indication of the available supply of illicitly manufactured fentanyl.
WHY IS THIS STUDY IMPORTANT?
The current overdose crisis in the US, driven in large part by opioid use, has evolved over the past two decades and is unlikely to be resolved soon. Opioid use has taken the lives of hundreds of thousands of people in the United States and is likely to adversely affect and end many more lives in the coming years. Concerted, multifaceted action is necessary to reduce the catastrophic toll of opioid-related deaths.
- LIMITATIONS
-
- The present study is not meant as an exhaustive exploration of the problem of overdose deaths in the US, and thus invariably omits some of the nuanced factors at play with this crisis.
NEXT STEPS
While the authors note many important next steps for addressing the current overdose crisis, they do not address how these steps might be implemented. This work falls to healthcare administrators, public health officials, policy makers, law enforcement, and the community.
Strategies are desperately needed that can prevent overdose and reduce the harm of substance use so that individuals might ultimately have the opportunity to pursue treatment. Though the benefit may be counterintuitive for many, harm reduction approaches such as safe injecting rooms and needle exchanges can greatly reduce the risk of overdose and the disease burden associated with addiction (e.g., reduced rates of Hepatitis C and HIV), while increasing drug users’ exposure to healthcare providers and educational materials, as well as their overall wellbeing. While harm reduction programs such as these are common in countries such as Australia, New Zealand, Canada, Holland, and in Scandinavia, the United States has been slow to adopt such approaches. In light of strong evidence supporting the effectiveness of these approaches, however, some United States cities are now considering adopting harm reduction strategies to fight the overdose crisis.
Strategies that help individuals regain their health and rebuild their lives are also needed to support individuals who have found their way to treatment, such as access to ongoing healthcare, education, and employment opportunities. It is critical too that all such interventions are subject to ongoing evaluation so they might be better adapted, improved and enhanced to ensure they are maximally effective.
BOTTOM LINE
- For individuals & families seeking recovery:If you or your loved one has an active opioid use disorder (i.e., currently using opioids), assume heroin is contaminated with fentanyl; reduce your risk of overdose by avoiding use while alone, and making sure associates have and know how to use naloxone (Narcan).
- For scientists: This opinion piece suggests numerous next steps for addressing the overdose crisis. Research assessing the efficacy and effectiveness of interventions such as starting patients on medications such as Suboxone in the emergency department, and integrating addiction care into general medical care is desperately needed, as is ongoing epidemiological research monitoring the crisis.
- For policy makers: Policies to increase the dissemination of, and access to evidence-based treatments, including medication for opioid use disorder would likely decrease the health, criminal justice, and financial burdens attributable to the current opioid crisis. Funding for research on clinical and recovery support services is needed to further improve outcomes for individuals with opioid use disorder. Moreover, legislation is needed that supports recovery and treatment provision, rather than punishment and criminalization of individuals addicted to drugs.
- For treatment professionals and treatment systems: Harm reduction approaches are a critical step in mitigating patient risk. All patients, especially those currently unwilling to stop opioid use, should be educated about the risks of fentanyl, and informed of available treatment options, including medications such as Suboxone.
CITATIONS
Dowell, D., Noonan, R. K., & Houry, D. (2017). Underlying Factors in Drug Overdose Deaths. Journal of the American Medical Association, 318(23), 2295-2296. doi:10.1001/jama.2017.15971

