Long-term change among people who inject drugs
Though individuals’ injection drug use patterns are known to change over time, most research to date has focused on short-term changes. This study sought to characterize longer-term patterns of injection drug use and identify factors related to change with the hope that this new knowledge can be used to improve treatments and public policies.
WHAT PROBLEM DOES THIS STUDY ADDRESS?
Individuals’ drug injection patterns are rarely stable. A number of previous studies have investigated drug use trajectories over short-term periods (~6 months) and have suggested that factors including intensity of drug injection, frequent non-injection drug use, polydrug use, alcohol use, age when injection drug use started, experiencing homelessness, incarceration, illegal income-generating activities, and treatment involvement all play an important role in influencing injection behavior change. At the same time, few studies have provided insight into the factors associated with patterns of injection drug use over multiple years, and only a small number of studies have examined longitudinal trajectories of injection drug use behavior over periods 10 years or greater. Such long-term studies can yield important information about the longitudinal characteristics of substance use disorder and injection drug use that could in turn help clinical scientists develop more effective treatments for substance use disorder. As such, this study sought to characterize long-term injection drug use trajectories and identify associated factors.
HOW WAS THIS STUDY CONDUCTED?
This was a 31 year-long observational, longitudinal study conducted in the Vancouver area in Canada, with participant assessments delivered every six months following study entry. The research team used existing data from 2,057 participants in two ongoing longitudinal studies of people who use drugs in Vancouver, Canada, the Vancouver Injection Drug Users Study (VIDUS), and the AIDS Care Cohort to evaluate Exposure to Survival Services (ACCESS).
Eligibility criteria for these studies included being at least 18 years of age at enrollment, residing in the Greater Vancouver area, and having injection drug use in the month prior to enrollment. In these studies, at baseline and every six months thereafter, participants completed an interviewer-administered questionnaire. Though the authors do not explicitly state it, it is inferred that participants in the VIDUS and ACCESS studies continue to do six-monthly follow-ups indefinitely. For individuals who were lost to follow-up or died, their first missed study visit was treated as the time of dropout. Nurses also assessed participants for various health conditions and obtained blood samples for HIV and hepatitis C testing, and HIV disease monitoring.
The authors only included participants who had at least four follow-up visits between 1 May 1996 and 30 November 2017 and reported taking illicit drugs via injection in the past six months at their baseline assessment.
Among 2,057 included participants, 1,309 (63.6%) were male, 1,195 (58.1%) identified as racially White (no other race/ethnicity information was provided), and the median age was 37 years. There were 740 participants (36%) who had ever been diagnosed with a mental health issue, and of those diagnosed, the most commonly reported diagnoses included depression (59.6%), anxiety (22.0%), bipolar disorder (13.0%), post-traumatic stress disorder (12.2%), and attention deficit disorder (8.4%).
Throughout the study period, 462 (22.5%) participants were lost to follow-up, and 495 participants were found to have died, including 103 (20.8%) HIV-related deaths, and 97 (19.6%) fatal overdose deaths.
Outcome Measures and Analysis
The main outcome of interest was self-reported injection drug use during the past six months (yes versus no). This was assessed by asking the participants: “In the last 6 months, when you were using, which of the following drugs did you inject?” The outcome variable was defined as ‘yes’ if participants indicated injecting substances including heroin alone, cocaine alone, heroin and cocaine, methamphetamine, heroin and crystal methamphetamine, crack cocaine, fentanyl powder/pills, benzodiazepines, prescription opioids, and any other specified drugs.
The authors also sought to evaluate whether specific baseline individual characteristics were associated with different injection drug use trajectories. Individual factors included: age; sex; education attainment; not being in a stable relationship; employment; and current housing status. Behavioral risk factors/outcomes and social exposures were categorized as yes versus no, and included: being attacked, assaulted, or suffered violence; drug dealing; sex work involvement; incarceration; and non-fatal overdose. All behavioral variables referred to the previous six months unless otherwise specified. Participants were also asked if they have ever been diagnosed with a mental health issue.
The authors used a statistical approach known as growth mixture modeling, which they used to identify distinctive sub-groups in their sample with similar patterns of injection drug use over time. They further evaluated whether these distinct sub-group patterns were associated with any of the assessed individual characteristics (e.g., primary substance taken, relationship status etc.). Information on participant fatality, including date and underlying causes of death, was obtained through a confidential data linkage with the British Columbia Vital Statistics Agency.
WHAT DID THIS STUDY FIND?
The authors identified five distinct injection drug use trajectory classes. They were, 1) ‘persistent injection’ (24.6%), 2) ‘persistent injection with late cessation’ (18.2%), 3) ‘gradual cessation’ (32.2%), 4) ‘early cessation with late relapse’ (11.0%), and 5) ‘early cessation’ (14.0%).
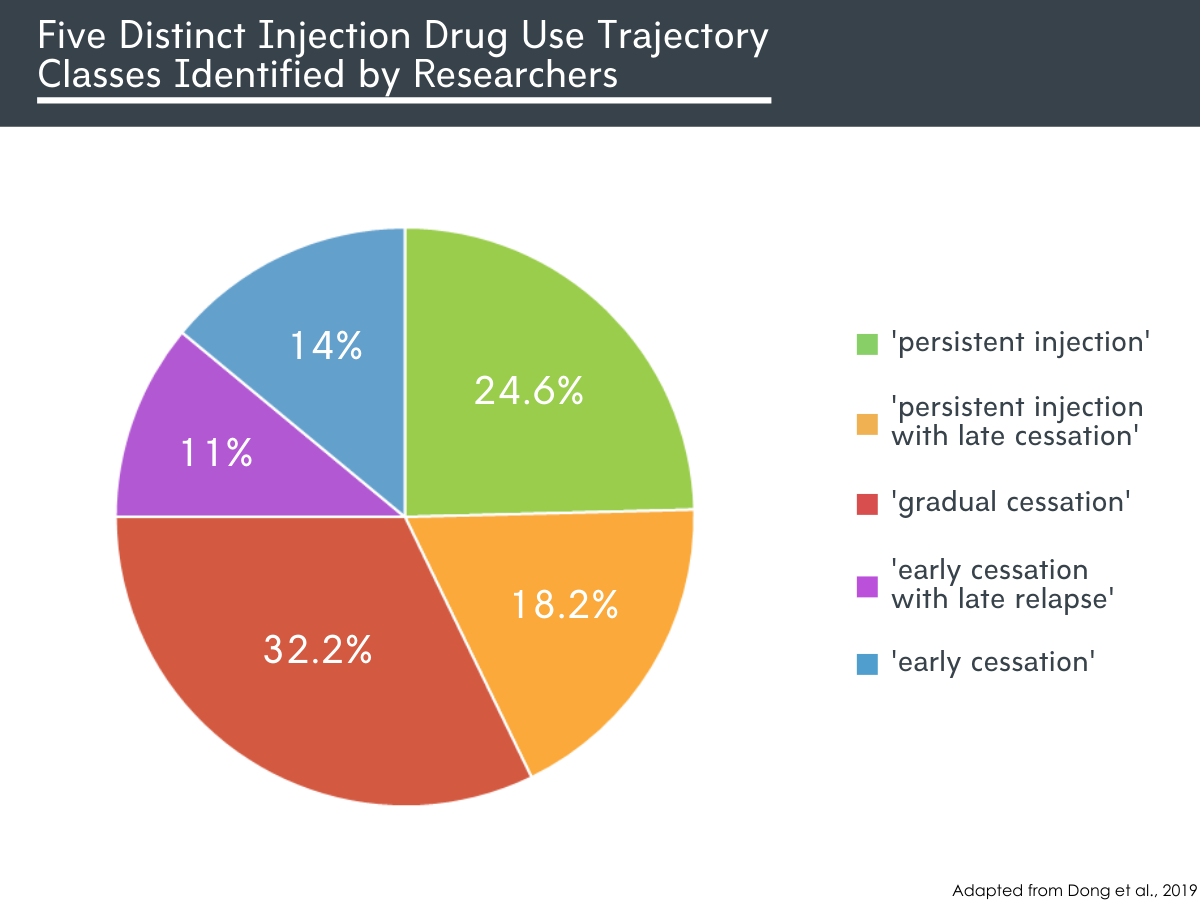
Figure 1.
Compared to the ‘early cessation’ group, participants of younger age were 2% more likely to be in the ‘persistent injection’ group and 3% more likely to be in the ‘persistent injection with late cessation’ group. Also, those endorsing being racially White were 53% more likely to fall into the ‘early cessation with late relapse’ versus ‘early cessation’ group. Further, those not in a stable relationship were 64% more likely to be in the ‘persistent injection’ group, 59% more likely to be in the ‘persistent injection with late cessation’ group, and 44% more likely to be in the ‘gradual cessation’ group.
Baseline substance use factors, including at least daily heroin injection and binge injection drug use (characterized by a ‘yes’ response to the question, “‘In the last six months, did you go on runs or binges, that is, when you injected drugs more than usual?”) were also found to be predictive of greater risk over the long term. Specifically, compared to the ‘early cessation’ group, participants who injected heroin daily were 41% more likely to be in the ‘persistent injection’ group, and 36% more likely to be in the ‘gradual cessation’ group. Moreover, participants who engaged in binge injection drug use at baseline were at 63% more likely to be in the ‘persistent injection’ group, and 77% more likely to be in the ‘gradual cessation’ group.
WHAT ARE THE IMPLICATIONS OF THE STUDY FINDINGS?
Dong and colleagues identified five distinct long-term patterns of injection drug use among people who inject drugs in Vancouver, Canada. Almost half the study participants had injected drugs for 15 years at study enrollment. Approximately one-quarter of the participants continued to inject drugs during the study period, and only a small portion of participants achieved sustained cessation of injection drug use by the end of their study participation. These trajectories displayed associations with several individual characteristics and drug use behaviors measured at baseline including younger age, not being in a stable relationship, and daily heroin injection and binge injection. It’s worth noting that, as the authors outlined, long-term studies of people who use injection drugs in the United States and Netherlands have shown a similar pattern of findings.
The authors’ findings are consistent with previous findings indicating that the majority of participants experienced at least one cessation and relapse episode during the study period. This is to be expected since substance use disorder is often characterized by attempts to stop use followed by return to use. For many individuals, achieving sustained remission from substance use disorder can take multiple attempts. Harm reduction initiative are an essential part of supporting these individuals to prevent overdose death and reduce disease exposure.
Given the large number of measures tested, it is perhaps surprising that the authors found so few demographic, social, and behavioral characteristics that were associated with specific injection drug use trajectories, meaning it’s hard to differentiate the different trajectory groups in terms of unique markers of long-term risk. Importantly, there are other key influential factors that were not specified and measured in this study. This might include individuals’ social network characteristics, and the availability of and access to other recovery capital.
Given the nature of the analyses, it is also not clear how some of these measures are related in time to injection trajectory. For instance, ‘not being in a relationship’ could be a cause, effect, or both, of ‘persistent injection’, ‘persistent injection with late cessation’, and ‘gradual cessation’. More research is needed to tease out the directional relationship between these factors.
Sadly, 495 participants were found to have died while enrolled in the ACCESS and VIDUS studies, which speaks to the high mortality rates among individuals using injection drugs. Of these deaths, 103 were HIV-related, and 97 were a result of fatal overdose. The fact more individuals died as a result of HIV than overdose highlights the fact that harms associated with injection drug use are often indirect, such as HIV or hepatitis C infection from sharing needles.
- LIMITATIONS
-
- Given the statistical approach utilized, temporal causality between measures could not be established. In other words, it is not clear whether certain measures were a cause or effect (or both) of associated measures.
- Many participants were lost to follow-up (22.5% of the sample). Though this is not uncommon in studies like this that longitudinally monitor individuals with substance use disorder, and the authors statistically controlled for drop out in their analyses, such a high dropout rate invariably reduces confidence in findings.
The authors noted the following limitations which are also important to emphasize:
- The use of self-report, especially for socially stigmatized and criminalized behaviors (e.g., illicit substance use), could introduce errors of recall and social desirability bias.
- The dichotomous variable of self-reported injection drug use (yes versus no) was used in the authors’ statistical models, therefore the identified trajectory classes could not differentiate between variability in frequency and quantity of injection drug use.
- There could be potentially important baseline characteristics that were not included when predicting trajectory groups. In other words, though the ACCESS and VIDUS studies collected many measures, many participant characteristics were invariably not assessed. For instance, the authors of this study were not able to report on factors such as abstinence motivation, self-efficacy, social network factors, and family support for recovery, or how these factors may have affected participant injection drug use trajectory.
- This study is not based on a random sample of people who inject drugs and was conducted in Vancouver, Canada, where the social–structural conditions (e.g., harm reduction strategies, attitudes towards injection drug use) could be different compared to other cities/countries. Therefore, these findings may not generalize to other samples in other regions.
BOTTOM LINE
- For individuals and families seeking recovery: The authors identified five distinct injection drug use change trajectories and several demographic, social, and behavioral characteristics associated with belongingness to these trajectories. At the same time, the findings are as notable for the many similarities between these change trajectory groups. Findings are heartening in that they show that the majority of the people monitored in this study (75.4%) were following some kind of injection drug use cessation trajectory, though some of these individuals may have ultimately been lost to follow-up or died. Only 24.6% of participants showed persistent injection drug use of the course of the study period. Other research has shown that recovery is likely among individuals who continue trying to achieve abstinence, even though it may take numerous recovery attempts.
- For treatment professionals and treatment systems: The authors identified five distinct injection drug use change trajectories and several demographic, social and behavioral characteristics associated with belongingness to these trajectories. At the same time, the findings are as notable for the many similarities between these change trajectory groups. Findings are heartening in that they show that the majority of the people monitored in this study (75.4%) were following some kind of injection drug use cessation trajectory, though some of these individuals may have ultimately been lost to follow-up or died. Only 24.6% of participants showed persistent injection drug use of the course of the study period. Other research has shown that recovery is likely among individuals who continue trying to achieve abstinence, even though it may take numerous recovery attempts. Treatment systems should utilize treatment structures that address the chronic, relapsing nature of substance use disorder, including adopting harm reduction approaches to buffer individuals against risk while they find their way to treatment.
- For scientists: The authors identified five distinct injection drug use change trajectories and several demographic, social and behavioral characteristics associated with belonging to these trajectories. At the same time, the findings are as notable for the many similarities between these change trajectory groups. Structural equation modelling studies that can parse out the temporal relationship between injection drug use trajectories and individual factors are needed to clarify Dong and colleagues’ findings. Future work should also explore psychological factors/characteristics associated with injection drug use trajectories. The findings from this study further highlight the importance of identifying targeted interventions for long-term injection drug use and the need to identify factors that support cessation and protect against relapse.
- For policy makers: The authors identified five distinct injection drug use change trajectories and several demographic, social and behavioral characteristics associated with belongingness to these trajectories. At the same time, the findings are as notable for the many similarities between these change trajectory groups. Findings are heartening in that they show that the majority of the people monitored in this study (75.4%) were following some kind of injection drug use cessation trajectory, though some of these individuals may have ultimately been lost to follow-up or died. Only 24.6% of participants showed persistent injection drug use of the course of the study period. Other research has shown that recovery is likely among individuals who continue trying to achieve abstinence, even though it may take numerous recovery attempts. Providing policy infrastructure that can help treatment systems address the chronic, relapsing nature of substance use disorder through harm reduction approaches, recovery support services, and longitudinal continuing care could greatly improve public safety and public health by reducing mortality, the spread of infectious disease (e.g., HIV, hepatitis C), and criminal justice costs.
CITATIONS
Dong, H., Hayashi, K., Singer, J., Milloy, M. J., DeBeck, K., Wood, E., & Kerr, T. (2019). Trajectories of injection drug use among people who use drugs in Vancouver, Canada, 1996-2017: Growth mixture modeling using data from prospective cohort studies. Addiction, 114(12), 2173-2186. doi: 10.1111/add.14756

