For Prisoners, Opioid Agonist Therapy Reduces Risks of Post-release Mortality by Up to 75%, So Why Do Some Patients Not Want It?
Opioid agonist therapy drastically reduces the risk of mortality after release from prison. Providers, however, reported that some patients prefer to cease treatment prior to release back into the community.
Why do some incarcerated individuals choose to initiate, continue, or discontinue life-saving treatment?
WHAT PROBLEM DOES THIS STUDY ADDRESS?
Incarceration is not uncommon among people with opioid use disorder. Australian policy has responded by making medication assisted treatments available in certain correctional jurisdictions. Since then patients have utilized a variety of treatment pathways including seeking opioid substitution treatment while in custody, discontinuation of treatment pre- or post-release into the community, or continuation of treatment post-release.
However, evidence based practice suggests that opioid agonist treatment in custody, with continued treatment in the community, significantly reduces post-release mortality by 75% and re-incarceration.
This study addressed the clinically important question of why patients choose to cease opioid agonist therapy while in custody. If clinicians can better understand patient’s ambivalence towards opioid agonist therapy, then they may be better able to attract and retain opioid dependent prisoners into treatment.
HOW WAS THIS STUDY CONDUCTED?
This qualitative study employed semi-structured interviews of 46 participants with a history of opioid dependence from seven correctional centers in New South Wales, Australia. All correctional centers in which recruitment was undertaken offered opioid agonist treatment.
In order to obtain a diversity of views on opioid agonist treatment in prisons, they included participants who initiated treatment in the community prior to incarceration, initiated treatment in custody, ceased treatment in custody, and not sought treatment while in custody. Over 2/3 of the sample were male and the average age was 35. Of the 27 participants currently in opioid agonist treatment, 26 were prescribed methadone, and one, buprenorphine–naloxone.
Specifically, the researchers examined:
- reasons for seeking opioid agonist treatment in custody
- preference to discontinue treatment post-release back into the community
- preference to continue treatment post-release
WHAT DID THIS STUDY FIND?
Several reasons were identified for not seeking opioid agonist treatment while in custody, seeking treatment while in custody, ending treatment prior to release into the community, and continuing treatment post-release.
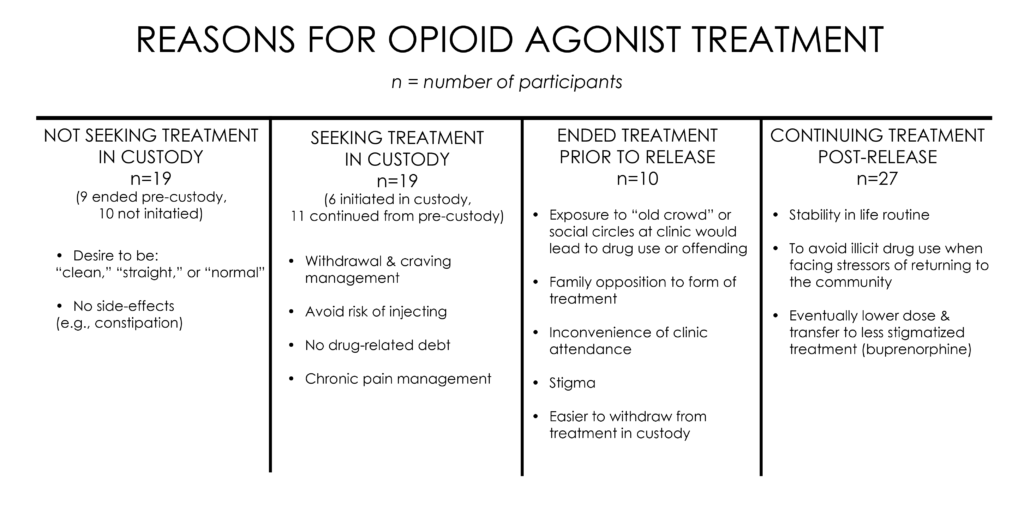
WHY IS THIS STUDY IMPORTANT?
For incarcerated individuals with an opioid use disorder, transitioning back into the community is a high risk time. Specifically, the first four weeks is associated with an increased risk for mortality.
Research with opioid dependent patients from the community has shown considerable ambivalence toward opioid agonist therapy. Little is known, however, about why people may terminate treatment prior to release from custody.
This study added to our knowledge-base by documenting reasons for opioid agonist treatment decisions among prisoners.
- LIMITATIONS
-
- This study is limited in its generalizability to incarcerated populations in the US. Australia has different policies and approaches than does the US to the treatment of substance use disorder in incarcerated populations which may be reflected in the patient’s decision making.
- Additionally, while a number of participants reported their intentions to cease opioid agonist treatment prior to or after release, the researchers do not know if they actually did.
NEXT STEPS
This qualitative study has generated unique data on patient perspectives of opioid agonist therapy in correctional settings. The next steps are to use the qualitative responses to inform a quantitative study, and determine the generalizability of the results to the larger population of incarcerated individuals. In addition, a longitudinal study will provide information on if the participants followed through with their treatment decisions, and how it affected their recovery.
BOTTOM LINE
- For individuals & families seeking recovery: While an inductive qualitative study such as this one does not lend itself to making specific recommendations from an evidence based framework or hypothesis test, the take home message is that if you are in custody, your decision to use opioid agonist treatment will have to balance the benefits of managing withdrawal, cravings, and reduced risk of drug injecting, with the risk of running into former peers at the clinic, opposition from others who disagree with your choice of treatment, and potential stigma.
- For Scientists: This study has laid some important ground work for understanding treatment decisions in incarcerated populations with an opioid use disorder. More work needs to be done on how clinicians can address patient treatment decisions that may put them at elevated risk for mortality or reoffending.
- For Policy makers: Given that some participants were reluctant to initiate or remain in opioid agonist treatment following release, there is a need for funding to study interventions to address post-release mortality risk. The authors suggest that take-home naloxone programs should be further explored for their utility in reducing post-release mortality.
- For Treatment professionals and treatment systems: Despite evidenced based guidelines for the use of opioid agonist treatment, your patient may be ambivalent about initiating or discontinuing this form of treatment. You may find your patient has similar concerns about the risks and benefits identified in this study regarding post-release treatment plans.
CITATIONS
Larney, S. Zador, D., Sindicich, N., & Dolan, K. (2016). A qualitative study of reasons for seeking and ceasing opioid substitution treatment in prisons in New South Wales, Australia. Drug and Alcohol Review, e-pub ahead of print.
Image Source: http://s.newsweek.com/sites/www.newsweek.com/files/styles/lg/public/2015/

