What is the Role of Mindfulness in Treatment of Substance Use Disorder?
Mindfulness training has received much attention in clinical research of late, which has generally supported its benefit for people suffering with anxiety and depression.
The primary goal of mindfulness training is to help the individual focus on his/her experience in the moment, without judging or acting based on emotional reaction.
Despite preliminary research that, as a personality trait, mindfulness predicts lower levels of substance use, we know very little about its potential role a teachable skill within the context of substance use disorder (SUD) treatment.
For example, by focusing on more neutral internal experiences compared to external cues, an individual with SUD may be able to increase acceptance of past negative actions or experiences. Mindfulness could also help those with SUD tolerate cravings and other unpleasant feelings without using substances, leading to gradual weakening of the link between negative emotion and substance use.
In order to test the potential benefits of mindfulness training, Bowen and colleagues compared mindfulness-based relapse prevention (MBRP) with standard relapse prevention (RP) and treatment as usual (TAU) among 286 participants, recruited from a continuing care SUD treatment program following participation in either a 30-day residential or 90-day intensive outpatient program.
- MBRP: The mindfulness-based relapse prevention intervention included eight weekly 2-hour sessions with 6 to 10 participants and two therapists. Consistent with other mindfulness training models, the therapists themselves had ongoing meditation practices. Each session had a specific topic (e.g., mindfulness in high-risk situations) and included 20-30 minutes of guided mediation.
- RP: The standard relapse prevention intervention was the same in length of time, format, size, and location as the MBRP intervention, though objectives of RP groups including addressing high-risk situations, behavioral coping, problem solving skills, and increasing self-efficacy.
- TAU: Treatment as usual was the program’s standard continuing care model, an abstinence-focused, 12-step approach; groups met 1 to 2 times per week for 1.5 hours.
All participants received treatment as usual (TAU), but mindfulness-based relapse prevention (MBRP) and standard relapse prevention (RP) patients were pulled from TAU groups during the 8 weeks they received one of the two special interventions. Patients were followed up at 3, 6, and 12 months after baseline.
Primary outcomes included:
A) probability of drug relapse (not including alcohol) and heavy drinking (4 or more drinks on one occasion for women, and 5 for men)
B) drug abstinence and no heavy drinking; also, among those who were not abstinent or had at least one heavy drinking day
C) frequency of substance use in the past 90 days was also examined as an outcome
There were no significant demographic differences between treatment groups at the start of treatment; however, treatment as usual (TAU) participants reported lower addiction severity on average than RP or MBRP participants.
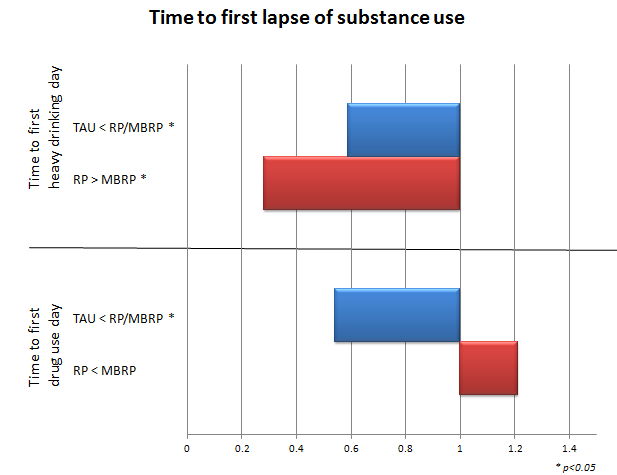
The authors first ran survival analyses to examine the risk of relapse to drug use and heavy drinking controlling for substance use severity, treatment history, and patient age. The outcomes here were determined by comparing the probability of drug relapse (or heavy drinking) in the treatment groups across the follow-up assessments (at 3-month, 6-month, and 12-month follow-ups). The probability of drug relapse for the combined group of RP/MBRP patients was 54% lower than TAU patients. Comparing only the active treatment conditions, probability of relapse for RP patients was 21% lower than MBRP patients. Regarding heavy drinking, the combined RP/MBRP group had a 59% lower probability of heavy drinking than TAU. RP and MBRP patients had similar probabilities of heavy drinking across study follow-ups.
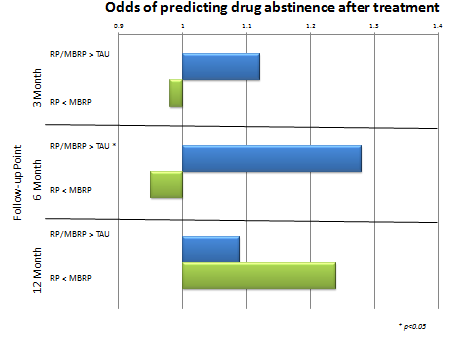
Regarding group differences in complete drug abstinence (i.e., no drug use whatsoever during that time) at each time point, RP/MBRP patients were 1.28 times more likely to be abstinent than TAU at 6-month follow-up, though there were no differences between RP/MBRP and TAU or between RP and MBRP at 3-month and 12-month follow-ups. Among those who used drugs at least once, MBRP patients had fewer drug use days than RP patients at 12-month follow-up only.
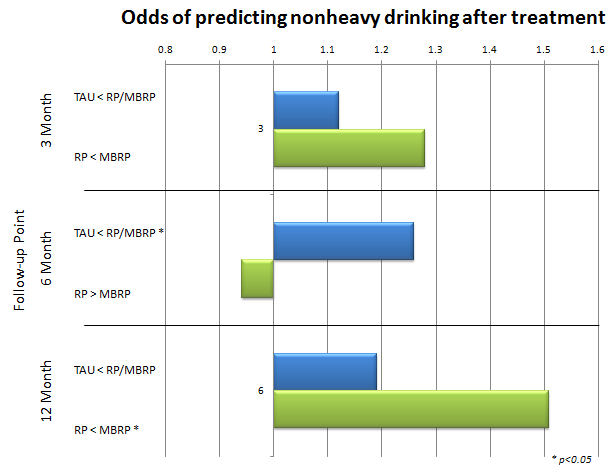
Regarding non-heavy drinking (never more than 3 drinks per day for women and 4 for men during that time), though there were no group differences at 3-month follow-up, standard relapse prevention (RP)/mindfulness-based relapse prevention (MBRP) participants were 1.26 times more likely to report only non-heavy drinking than treatment as usual (TAU) participants at 6-month follow-up.
At 12-month follow-up, although similar proportions of RP/MBRP and TAU participants reported non-heavy drinking, MBRP participants were 1.51 times more likely than the RP group to report only non-heavy drinking.
Among those who had at least one heavy drinking day, the combined MBRP/RP group had fewer heavy drinking days than TAU only at 6 months. Authors did not find any other differences between the combined MBRP/RP group and TAU or between MBRP and RP.
IN CONTEXT
Beginning with its inclusion in dialectical behavior therapy treatments in the early 1990s, mindfulness-based strategies have grown in popularity among Western models of psychological intervention and well-being, including in the addiction field.
Following emerging evidence that mindfulness-based treatments can help individuals struggling with depression and anxiety, and correlational studies showing a relationship between mindfulness and less substance use, Bowen and colleagues tested the efficacy of mindfulness-based relapse prevention (MBRP) using a strong research design in almost 300 patients with substance use disorder.
Overall, the authors’ findings suggest mindfulness-based relapse prevention (MBRP) may have promise as an substance use disorder treatment. Yet this study did not demonstrate a clear advantage for MBRP relative to standard relapse prevention (RP). Mindfulness-based treatments require the therapists have their own meditation practice, and receive additional training in the delivery of the therapy, which takes substantial time and effort.
The modest abstinence-related benefit of mindfulness-based relapse prevention (MBRP) relative to the more widespread cognitive-behavioral model may not yet justify the potential extra time and money needed to provide therapists with this type of training. Where there may be advantages for MBRP relative to standard relapse prevention (RP), these may not emerge until well after patients received the treatment.
The authors’ hypothesis — that delayed MBRP effects might be the result of improved ability over time to recognize and tolerate discomfort associated with craving or negative emotion — is certainly an interesting one, and could be tested in a future longitudinal research study perhaps using ecological momentary assessments that can capture cravings, urges, and use of MBRP strategies in real-time.
NEXT STEPS
Another study would be to test the effect of mindfulness-based relapse prevention (MBRP) for patients when they are allowed to make a choice between standard relapse prevention (RP) vs. mindfulness-based relapse prevention (MBRP) vs. treatment as usual (TAU), because it may offer a compelling choice for some patients, such individuals may use it more and benefit it from it to a greater degree.
CITATIONS
Bowen, S., Witkiewitz, K., Clifasefi, S. L., Grow, J., Chawla, N., Hsu, S. H., … & Larimer, M. E. (2014). Relative efficacy of mindfulness-based relapse prevention, standard relapse prevention, and treatment as usual for substance use disorders: a randomized clinical trial. JAMA psychiatry, 71(5), 547-556.

