l
Many individuals with substance use disorder in United States do not access care; less than 10% of people with a substance use disorder receive any treatment. Due to substance use disorder and crime often being associated, criminal-legal systems have implemented efforts to refer offenders to treatment, including through diversion programs. Concurrently, programs that reduce the harms of drug use (including syringe service programs) are another avenue through which people who use drugs have been linked to treatment. A better understanding of the relative utility of these different approaches for linking people to treatment can help inform public health policies and resource allocation. This study compared rates of substance use disorder treatment uptake between people who use drugs who had contact with either syringe exchange programs or the criminal legal system.
This was a cross-sectional study of 770 adults who used illicit drugs in the past 30 days living in San Francisco, California. Participants were recruited through outreach settings (e.g., homeless encampments) and not directly from syringe service programs or criminal justice settings (e.g., prisons). Recent (i.e., past 3-month) criminal legal system involvement and syringe service program usage was determined by face-to-face interview questions. For example, “In the past 3 months, how many times have you been to a needle exchange?”, and “In the past 3 months, how many times were you stopped by the police (even if it didn’t lead to arrest or further legal consequences)?” The outcome of this study was the uptake of any substance use disorder treatment in the past 3 months, including medication treatment (e.g., methadone), outpatient treatment, inpatient treatment (e.g., hospitalization), recovery residence stays, counseling from physicians, and mutual-help groups such as Narcotics Anonymous.
It is worth noting the lack of specificity in these measures can impact results. For example, not all routine police encounters result in referral to substance use treatment, meaning that more frequent police stops do not necessarily reflect more opportunities to be referred to treatment. This is especially relevant as 72% of the participants were experiencing homelessness and the study was conducted from 2023-2024 in San Francisco. During this time, California had enacted aggressive policies to remove homeless encampments, which likely increased interactions between homeless participants and law enforcement. In addition, the homeless population in California may differ from homeless populations elsewhere in the United States. Results should be considered with these limitations in mind.
Most participants reported recent syringe service program use (78%) despite only 34% reporting any recent injection drug use. Almost 50% of participants reported any involvement with the criminal justice system (the most common involvement was police stops [42%]). The most used illicit drugs were methamphetamine (82%) and cocaine (82%).
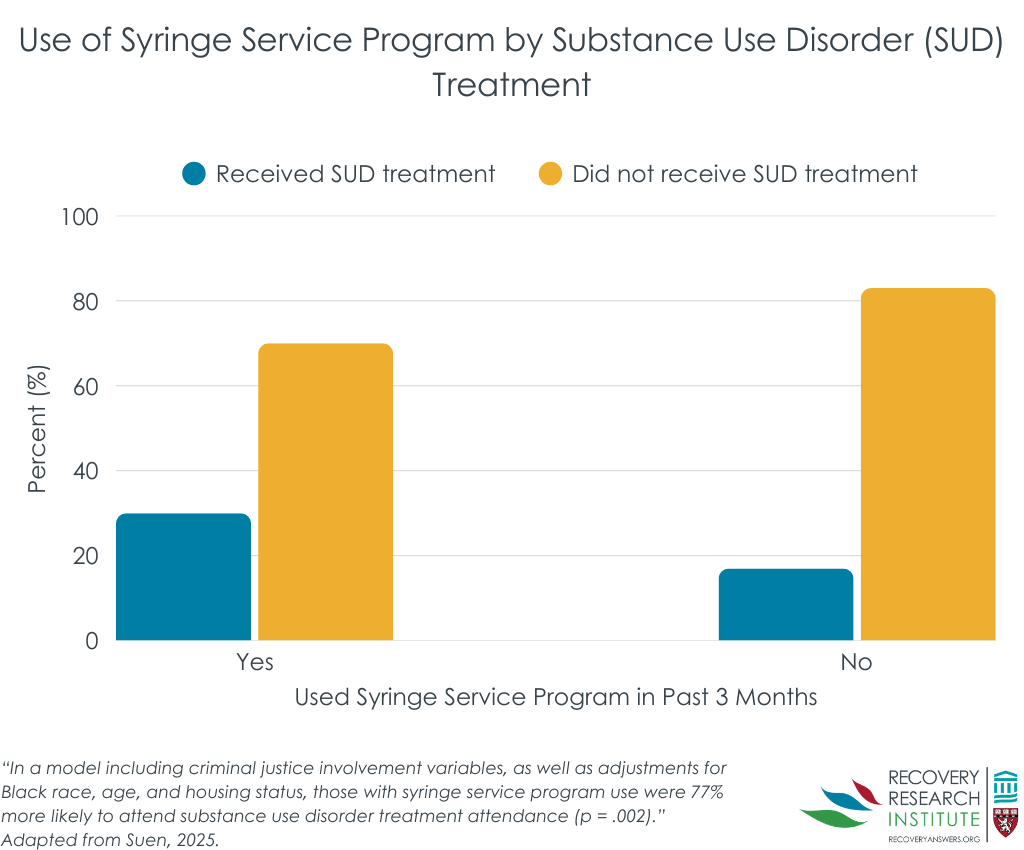
Only 27% of participants reported any substance use disorder treatment engagement in the past 3 months. However, controlling for criminal-legal involvement as well as race, age, and housing status, participants who recently used syringe service programs were 77% more likely to report recent substance use disorder treatment engagement than those who did not use syringe service programs (see graph below). More frequent syringe service program use was not associated with increased likelihood of substance use disorder treatment engagement. In contrast, participants who reported recent involvement with the criminal justice system were no more likely to have received treatment than those who had not interacted with the criminal justice system.
This study underscores the need for research on the impact of different programs on substance use disorder treatment engagement. The study found that participants who interfaced with syringe service programs (but not the criminal justice system) were more likely to receive treatment and recovery support services. However, results may have been impacted by the limitations of the study. Importantly, the cross-sectional nature of the study makes it difficult to determine if involvement with the syringe service program impacted later substance use disorder treatment engagement or vice versa. That is, treatment programs may be referring to syringe service programs, rather than the reverse.
Also, treatment referrals may occur at multiple time points during justice system interactions, so limiting measurement of criminal justice involvement to past 3-month interactions may have restricted the measured opportunities for referral. Indeed, referral programs within justice contexts can be helpful and can help reduce future justice involvement. Finally, syringe service program usage was associated with substance use treatment engagement, but it is possible that the short time frame obscured meaningful nuances. That is, the success of syringe service programs in referring people to treatment may be because clients come to trust program personnel through longstanding working relationships. The 3-month timeframe used in the current study may have been too short to capture changes in treatment perception and utilization. Thus, the treatment linkage rate from syringe service programs may have been even larger if researchers used a longer timeframe.
Syringe service programs may be a useful way to facilitate referral to treatment among those with substance use disorder, but more research is needed given the cross-sectional design used here.
Suen, L. W., Megerian, C. E., Browne, E. N., Chung, E. O., Akiba, C. F., Williams, J., Humphrey, J. L., Wenger, L. D., Ray, B., Lambdin, B. H.,& Kral, A. H. (2025). Linkage to substance use disorder treatment through syringe services programs and the criminal legal system: A cross-sectional study. American Journal of Preventive Medicine, 70(2). doi: 10.1016/j.amepre.2025.108150.
l
Many individuals with substance use disorder in United States do not access care; less than 10% of people with a substance use disorder receive any treatment. Due to substance use disorder and crime often being associated, criminal-legal systems have implemented efforts to refer offenders to treatment, including through diversion programs. Concurrently, programs that reduce the harms of drug use (including syringe service programs) are another avenue through which people who use drugs have been linked to treatment. A better understanding of the relative utility of these different approaches for linking people to treatment can help inform public health policies and resource allocation. This study compared rates of substance use disorder treatment uptake between people who use drugs who had contact with either syringe exchange programs or the criminal legal system.
This was a cross-sectional study of 770 adults who used illicit drugs in the past 30 days living in San Francisco, California. Participants were recruited through outreach settings (e.g., homeless encampments) and not directly from syringe service programs or criminal justice settings (e.g., prisons). Recent (i.e., past 3-month) criminal legal system involvement and syringe service program usage was determined by face-to-face interview questions. For example, “In the past 3 months, how many times have you been to a needle exchange?”, and “In the past 3 months, how many times were you stopped by the police (even if it didn’t lead to arrest or further legal consequences)?” The outcome of this study was the uptake of any substance use disorder treatment in the past 3 months, including medication treatment (e.g., methadone), outpatient treatment, inpatient treatment (e.g., hospitalization), recovery residence stays, counseling from physicians, and mutual-help groups such as Narcotics Anonymous.
It is worth noting the lack of specificity in these measures can impact results. For example, not all routine police encounters result in referral to substance use treatment, meaning that more frequent police stops do not necessarily reflect more opportunities to be referred to treatment. This is especially relevant as 72% of the participants were experiencing homelessness and the study was conducted from 2023-2024 in San Francisco. During this time, California had enacted aggressive policies to remove homeless encampments, which likely increased interactions between homeless participants and law enforcement. In addition, the homeless population in California may differ from homeless populations elsewhere in the United States. Results should be considered with these limitations in mind.
Most participants reported recent syringe service program use (78%) despite only 34% reporting any recent injection drug use. Almost 50% of participants reported any involvement with the criminal justice system (the most common involvement was police stops [42%]). The most used illicit drugs were methamphetamine (82%) and cocaine (82%).
Only 27% of participants reported any substance use disorder treatment engagement in the past 3 months. However, controlling for criminal-legal involvement as well as race, age, and housing status, participants who recently used syringe service programs were 77% more likely to report recent substance use disorder treatment engagement than those who did not use syringe service programs (see graph below). More frequent syringe service program use was not associated with increased likelihood of substance use disorder treatment engagement. In contrast, participants who reported recent involvement with the criminal justice system were no more likely to have received treatment than those who had not interacted with the criminal justice system.

This study underscores the need for research on the impact of different programs on substance use disorder treatment engagement. The study found that participants who interfaced with syringe service programs (but not the criminal justice system) were more likely to receive treatment and recovery support services. However, results may have been impacted by the limitations of the study. Importantly, the cross-sectional nature of the study makes it difficult to determine if involvement with the syringe service program impacted later substance use disorder treatment engagement or vice versa. That is, treatment programs may be referring to syringe service programs, rather than the reverse.
Also, treatment referrals may occur at multiple time points during justice system interactions, so limiting measurement of criminal justice involvement to past 3-month interactions may have restricted the measured opportunities for referral. Indeed, referral programs within justice contexts can be helpful and can help reduce future justice involvement. Finally, syringe service program usage was associated with substance use treatment engagement, but it is possible that the short time frame obscured meaningful nuances. That is, the success of syringe service programs in referring people to treatment may be because clients come to trust program personnel through longstanding working relationships. The 3-month timeframe used in the current study may have been too short to capture changes in treatment perception and utilization. Thus, the treatment linkage rate from syringe service programs may have been even larger if researchers used a longer timeframe.
Syringe service programs may be a useful way to facilitate referral to treatment among those with substance use disorder, but more research is needed given the cross-sectional design used here.
Suen, L. W., Megerian, C. E., Browne, E. N., Chung, E. O., Akiba, C. F., Williams, J., Humphrey, J. L., Wenger, L. D., Ray, B., Lambdin, B. H.,& Kral, A. H. (2025). Linkage to substance use disorder treatment through syringe services programs and the criminal legal system: A cross-sectional study. American Journal of Preventive Medicine, 70(2). doi: 10.1016/j.amepre.2025.108150.
l
Many individuals with substance use disorder in United States do not access care; less than 10% of people with a substance use disorder receive any treatment. Due to substance use disorder and crime often being associated, criminal-legal systems have implemented efforts to refer offenders to treatment, including through diversion programs. Concurrently, programs that reduce the harms of drug use (including syringe service programs) are another avenue through which people who use drugs have been linked to treatment. A better understanding of the relative utility of these different approaches for linking people to treatment can help inform public health policies and resource allocation. This study compared rates of substance use disorder treatment uptake between people who use drugs who had contact with either syringe exchange programs or the criminal legal system.
This was a cross-sectional study of 770 adults who used illicit drugs in the past 30 days living in San Francisco, California. Participants were recruited through outreach settings (e.g., homeless encampments) and not directly from syringe service programs or criminal justice settings (e.g., prisons). Recent (i.e., past 3-month) criminal legal system involvement and syringe service program usage was determined by face-to-face interview questions. For example, “In the past 3 months, how many times have you been to a needle exchange?”, and “In the past 3 months, how many times were you stopped by the police (even if it didn’t lead to arrest or further legal consequences)?” The outcome of this study was the uptake of any substance use disorder treatment in the past 3 months, including medication treatment (e.g., methadone), outpatient treatment, inpatient treatment (e.g., hospitalization), recovery residence stays, counseling from physicians, and mutual-help groups such as Narcotics Anonymous.
It is worth noting the lack of specificity in these measures can impact results. For example, not all routine police encounters result in referral to substance use treatment, meaning that more frequent police stops do not necessarily reflect more opportunities to be referred to treatment. This is especially relevant as 72% of the participants were experiencing homelessness and the study was conducted from 2023-2024 in San Francisco. During this time, California had enacted aggressive policies to remove homeless encampments, which likely increased interactions between homeless participants and law enforcement. In addition, the homeless population in California may differ from homeless populations elsewhere in the United States. Results should be considered with these limitations in mind.
Most participants reported recent syringe service program use (78%) despite only 34% reporting any recent injection drug use. Almost 50% of participants reported any involvement with the criminal justice system (the most common involvement was police stops [42%]). The most used illicit drugs were methamphetamine (82%) and cocaine (82%).
Only 27% of participants reported any substance use disorder treatment engagement in the past 3 months. However, controlling for criminal-legal involvement as well as race, age, and housing status, participants who recently used syringe service programs were 77% more likely to report recent substance use disorder treatment engagement than those who did not use syringe service programs (see graph below). More frequent syringe service program use was not associated with increased likelihood of substance use disorder treatment engagement. In contrast, participants who reported recent involvement with the criminal justice system were no more likely to have received treatment than those who had not interacted with the criminal justice system.

This study underscores the need for research on the impact of different programs on substance use disorder treatment engagement. The study found that participants who interfaced with syringe service programs (but not the criminal justice system) were more likely to receive treatment and recovery support services. However, results may have been impacted by the limitations of the study. Importantly, the cross-sectional nature of the study makes it difficult to determine if involvement with the syringe service program impacted later substance use disorder treatment engagement or vice versa. That is, treatment programs may be referring to syringe service programs, rather than the reverse.
Also, treatment referrals may occur at multiple time points during justice system interactions, so limiting measurement of criminal justice involvement to past 3-month interactions may have restricted the measured opportunities for referral. Indeed, referral programs within justice contexts can be helpful and can help reduce future justice involvement. Finally, syringe service program usage was associated with substance use treatment engagement, but it is possible that the short time frame obscured meaningful nuances. That is, the success of syringe service programs in referring people to treatment may be because clients come to trust program personnel through longstanding working relationships. The 3-month timeframe used in the current study may have been too short to capture changes in treatment perception and utilization. Thus, the treatment linkage rate from syringe service programs may have been even larger if researchers used a longer timeframe.
Syringe service programs may be a useful way to facilitate referral to treatment among those with substance use disorder, but more research is needed given the cross-sectional design used here.
Suen, L. W., Megerian, C. E., Browne, E. N., Chung, E. O., Akiba, C. F., Williams, J., Humphrey, J. L., Wenger, L. D., Ray, B., Lambdin, B. H.,& Kral, A. H. (2025). Linkage to substance use disorder treatment through syringe services programs and the criminal legal system: A cross-sectional study. American Journal of Preventive Medicine, 70(2). doi: 10.1016/j.amepre.2025.108150.
151 Merrimac St., 4th Floor. Boston, MA 02114