E-Interventions for Alcohol Increase Reach, But Do They Work?
E-Interventions include web-based resources, Smartphone apps, & interactive voice response, where automated telephone messages and prompts are offered in response to patients’ reported functioning (e.g., craving, recent use, motivation).
WHAT PROBLEM DOES THIS STUDY ADDRESS?
Electronic interventions (e-interventions) to address alcohol and other drug use are becoming increasingly common ways of:
a) preventing onset of substance use disorder
b) enhancing the reach of substance use disorder treatment to improve access
c) extending the benefit of treatment as a continuing care intervention (e.g., they can help individuals maintain abstinence after treatment)
Reviews and meta-analyses (which analyze the results of several studies at the same time) suggest e-interventions can help reduce drinking, with one meta-analysis showing a reduction of 26g of alcohol per week, the equivalent of about 2 standard drinks in the U.S. However, the substantial majority of these studies focus on short-term outcomes (less than 6 months). Less is known about how long these effects can last.
In the current study, Dedert et al. analyzed the effects of e-interventions for alcohol misuse and alcohol use disorder at 6 months and beyond.
HOW WAS THIS STUDY CONDUCTED?
Authors analyzed 28 randomized controlled trials conducted between 2000 and 2014 that compared e-interventions for alcohol misuse or alcohol use disorder with an inactive intervention (e.g., educational materials only) and had a follow-up assessment at least 6 months after the intervention was delivered. They used a standardized metric of grams of pure alcohol per week regarding alcohol consumption; they also analyzed changes in binge drinking and whether participants met specific drinking limit guidelines (e.g., NIAAA guidelines of 14 or fewer drinks per week not to exceed 3 drinks on any given day for men, and 7 or fewer drinks per week, not to exceed 2 drinks on any given day, for women).
The study examined findings separately for college student and non-college student adult samples If there were three or more studies for a particular outcome within one of these participant groups at one point in time (e.g., binge drinking in college students at 6-month follow-up), authors conducted a meta-analysis. They also rated each study with respect to risk for bias (low, medium, high), which is synonymous with internal validity, or the “extent to which the results of the study are correct for the circumstances being studied”. One element, for example, that factors into risk of bias is whether the study used valid and reliable measures to assess the outcome (see here). When possible, they compared results when including and excluding studies with high risk of bias.
WHAT DID THIS STUDY FIND?
Of the 28 studies, 14 examined college students and 14 examined non-college adults. The majority of the e-interventions were brief (e.g., 1 session) and delivered via the Internet. Of these 28, 19 were a single session, lasting 10 minutes, on average, for adult samples, and 25 minutes, on average, for college samples.
Regarding alcohol consumption in adults, using only studies with low/moderate risk of bias, authors found a statistically significant, but small effect of e-interventions, a reduction in about 1 drink per week (using the United States standardized 14g of pure alcohol per drink) at 6 months.
Including studies with high risk of bias yielded no difference between the e-intervention and comparison group & no effect of e-interventions at 12 months.
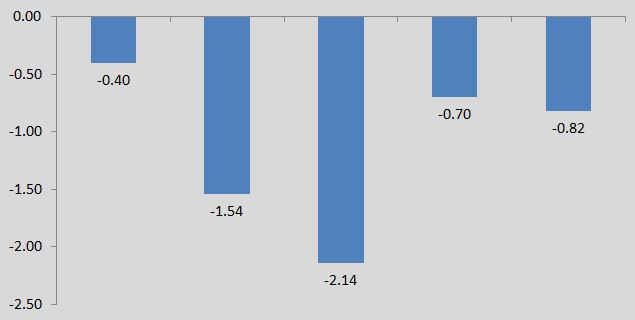
Graphical depiction of the difference between intervention and comparison in terms of their change from baseline to 6-month follow-up for both adult non-college students.
In these figures, negative values indicate a reduction in drinking relative to comparison (e.g., -1 means that individuals receiving the intervention had a reduction of 1 standard U.S. drink, or 14g or pure alcohol, relative to the comparison group) and positive values an increase in drinking relative to comparison.
***Note: In a meta-analysis, studies with larger samples (sample size is not shown here), are weighted more heavily in the calculations (i.e., have a greater contribution).
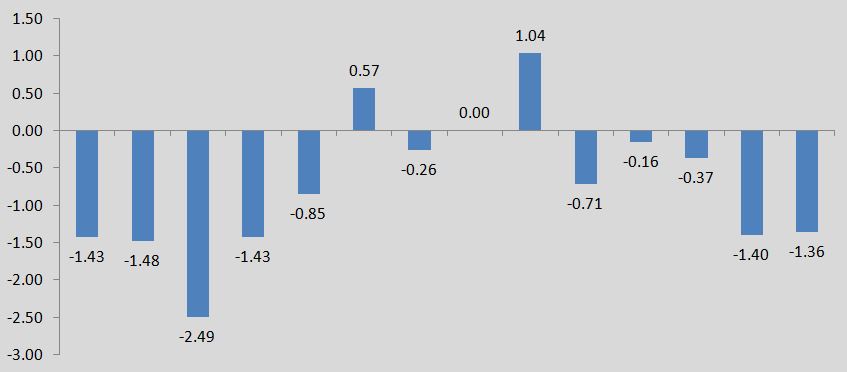
Graphical depiction of the difference between intervention and comparison in terms of their change from baseline to 6-month follow-up for both adult college students, including only studies with low and moderate levels of risk of bias.
Regarding whether the e-interventions led to changes in meeting drinking limit guidelines, the interventions were not statistically different from comparison groups at 6 months; none reported outcomes at 12 months. Regarding binge drinking, there were similar effects for e-interventions and comparison groups at 6 months for college students, and for adults also among two studies only (a meta-analysis was not conducted).
Although a meta-analysis was not conducted for individuals with likely alcohol use disorder (e.g., sampled from individuals who completed alcohol use disorder (AUD) treatment), authors reviewed three trials meeting study criteria.
They found that a trial of phone counseling plus computerized feedback, and a trial of interactive voice response produced similar 12 month and 6 month drinking outcomes, respectively, relative to comparison. However, participants assigned to engage with a mobile application after residential treatment that included several tools such as ongoing risk assessments, alerts when participants were located near high-risk targets and areas (e.g., bars), and guided relaxation exercises, were two times more likely to be abstinent at 12-month follow-up relative to those receiving continuing care as usual (e.g., “aftercare” groups; see here for the original study).
This study suggests that, among individuals with other forms of harmful or hazardous alcohol use (e.g., heavy drinkers), the effects of the majority of e-interventions may not be sustainable at 6 months or more beyond the initial intervention.
Ongoing access to and engagement with these e-interventions in the form of booster sessions (e.g., re-engaging with materials 3 months after initial receipt of the intervention) may be needed to maintain gains.
WHY IS THIS STUDY IMPORTANT
Alcohol is responsible for 1 in 10 deaths of people of working age in the U.S. & is one of the foremost contributors to the national burden of disease and disability.
It is crucial, therefore, to understand the effectiveness of brief, electronic interventions due to their potential to improve the reach of alcohol-related public health interventions.
The current study adds to that understanding with its focus on longer-term effects (6 months and beyond).
For individuals with alcohol use disorder (AUD), the use of a continuing care intervention which included multiple components in a mobile format along with additional support from a counselor as needed resulted in a doubling of abstinence rates 12 months after discharge from residential treatment (4 months after no longer having access to the mobile application). If mobile interventions are to work, it is likely that intensive e-interventions made available over several months or more are needed to produce meaningful and lasting changes in alcohol use.
- LIMITATIONS
-
- The meta-analytic approach of this study was both a strength and limitation. A meta-analysis helps answer broad questions about a particular area like e-interventions across many studies; it may miss, however, nuanced issues about an intervention that could have important public health and clinical implications (e.g., that certain types of interventions work better than others). It is important to note the current study was characterized by a series of meta-analyses and authors did not – or were not able to – analyze whether e-interventions may be more effective over time for certain subgroups apart from college versus non-college samples (which the current study analyzed separately), or that certain types of e-interventions may be more effective than others.
NEXT STEPS
These results were similar to another meta-analysis that analyzed the benefit provided by offering individuals a brief assessment of their drinking along with information about how the amount, frequency, and intensity of one’s drinking compares to his/her peers (i.e., normative feedback). They considered several ways in which this assessment and feedback could be delivered including in-person, standard (non-electronic) mail, and via the Internet.
They also found this assessment and feedback intervention produced small effects, and only for some outcomes (see here). It is important to note that in one of the successful trials that was reviewed in the current study, college students received a 1-month booster intervention (intended to “boost” the reduced effect of the e-intervention over time; see here). Repeat access and engagement may produce better long-term outcomes, though this hypothesis requires further examination in future investigations.
Future work may also investigate whether a reduction in one drink (down from an initial 10 or more drinks per week) actually has a real-world positive impact on one’s functioning at school, work, or in the individual’s relationships.
BOTTOM LINE
- For individuals & families seeking recovery: E-interventions for drinking have been tested mostly on those whose drinking may not reach the level of alcohol use disorder. More research is needed before e-interventions can be recommended as a way to help you reduce or quit drinking.
- For scientists: This series of meta-analyses suggests e-interventions can lead to very modest benefits (reduction of about 1 drink per week) among individuals with hazardous or risky drinking at 6-month follow-up. This may be too small a reduction to make a real difference in actual harms and hazards. Future work could test whether a) such a reduction actually is associated with improved functioning, and b) addition of booster sessions could improve long-term benefit.
- For policy makers: Cost-benefit analyses are needed to determine whether e-interventions are worthwhile investments. Given the current research, the benefit appears to be very small at least with respect to brief interventions. Even with only a small benefit, however, the substantial reach and potential accessibility of e-interventions could mean that even small effects might have a broad public health impact. This area merits more work on benefits and costs.
- For treatment professionals and treatment systems: It is possible that e-interventions designed specifically for individuals with alcohol use disorder (as in Gustafson et al.’s study mentioned in Treatment and Recovery Implications above; see here) can improve treatment outcomes, particularly as continuing care strategies. However, practical strategies for accessing and implementing them in the community have not yet been investigated.
CITATIONS
Dedert, E. A., McDuffie, J. R., Stein, R., McNiel, J. M., Kosinski, A. S., Freiermuth, C. E., . . . Williams, J. W., Jr. (2015). Electronic Interventions for Alcohol Misuse and Alcohol Use Disorders: A Systematic Review. Ann Intern Med, 163(3), 205-214. doi:10.7326/m15-0285

