WHAT PROBLEM DOES THIS STUDY ADDRESS?
The number of states in the US that have legalized the recreational use of cannabis for adults is growing. As of 2025, 24 states and Washington, DC have legalized sales, resulting in greater access to cannabis, even among adolescents for whom sales are illegal, as well as sales of products of very high THC potency. Starting use of cannabis early in life and heavy use of cannabis with a high potency of tetrahydrocannabinol (THC; the primary psychoactive compound in cannabis) can increase risk for a variety of cognitive deficits and mental health conditions, including depression, suicidal behavior, and psychosis. People with psychiatric conditions or who are at greater risk for psychiatric conditions may be especially vulnerable to cannabis use, given it can worsen existing symptoms or bring dormant symptoms on sooner. It is unclear how legalization of recreational cannabis sales has influenced rates of cannabis use and cannabis-related disorders among this population. This study examined whether legalizing recreational sales of cannabis in Massachusetts was associated with increases in cannabis use and cannabis-related disorders across age groups among people presenting to a psychiatric emergency service.
HOW WAS THIS STUDY CONDUCTED?
This study used electronic health records from patients presenting to a psychiatric emergency service in Boston, Massachusetts to examine the effects of legalizing recreational sales of cannabis on cannabis use and cannabis-related disorders across age groups. The primary outcomes of interest were cannabis use in the last month, as measured by a positive urine test for THC, and cannabis-related disorders, as measured by the clinician-determined ICD-10 diagnostic criteria for cannabis abuse, cannabis dependence, and clinically significant cannabis use. The diagnosis of clinically significant cannabis use was given when the provider has determined that cannabis use was contributing significantly to the patients’ psychiatric symptoms. Patients were given a toxicology urine screen if they presented to the emergency service with serious trauma, were being held for an involuntary psychiatric evaluation, presented with a primary substance-use related complaint, or upon the recommendation of the provider. Data was collected between January 1, 2017 and December 31, 2019, which captures the time from before recreational sales of cannabis was legalized (i.e., “pre-commercialization, Jan. 1, 2017 – Nov. 19, 2018) to after (i.e., post-commercialization, Nov. 20, 2018 – Dec. 31, 2019), as the first day of legal retail cannabis sales in MA was Nov. 20, 2018. For the analyses, patients were grouped by age: adolescents aged 12-17 years; young adults aged 18-25; adults aged 26-49; and older adults aged 50-70. The statistical analyses adjusted for the covariates of sex, race, and ethnicity. The study also examined whether results held up when controlling for a series of potential confounding variables (using a method called propensity score matching). Such statistical adjustments help to isolate the effect of interest – i.e., whether recreational sales of cannabis are independently related to cannabis use and cannabis-related outcomes in psychiatric emergency room patients. Analyses included data from a total of 7,350 electronic health records.
Of note, despite accounting for many alternative explanations by controlling for demographic factors, because this research design is correlational and not experimental, the researchers cannot examine if the associations between legalization of recreational cannabis sales and cannabis outcomes are causal. The research design also does not allow the researchers to separate the effects of legalizing medical marijuana, which occurred in 2013 in MA, from the effects of legalizing recreational sales analyzed in the current study. Future research that examines effects of both types of legalization across a greater period of time would be needed to disentangle these effects.
WHAT DID THIS STUDY FIND?
Overall, rates of cannabis use among psychiatric emergency room patients increased from 32% during the pre-commercialization period to 36% during the post-commercialization period. However, there were no changes in cannabis-related disorders from pre- to post-commercialization in the overall sample.
Associations between legalization of recreational cannabis sales and cannabis outcomes varied by age (graph below). The largest increase in rates of cannabis use was found for adolescents aged 12-17, with an increase from 5% during the pre-commercialization period to 17% during the post-commercialization period. For adults aged 26-49, there was also an increase in rates of cannabis use but it was more modest, increasing from 38% during the pre-commercialization period to 43% during the post-commercialization period. There were no differences in cannabis use rates between pre- and post-commercialization for young adults aged 18-25 and older adults aged 50-70.

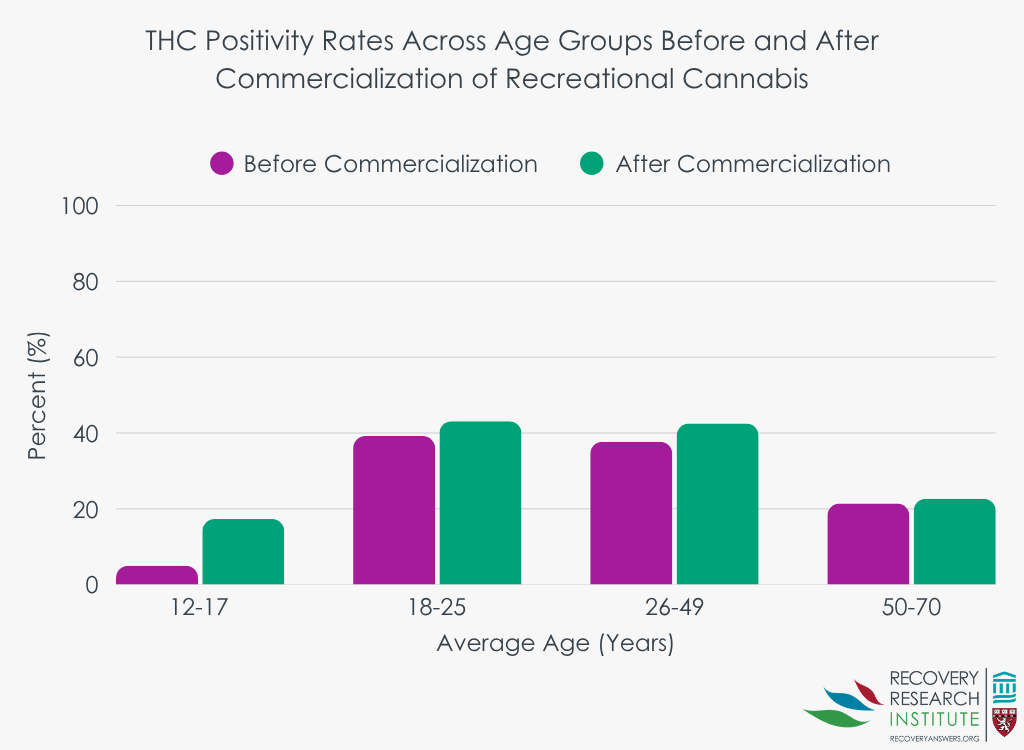
Adolescents were the only age group to have an increase in cannabis-related disorders, with an increase from 3% during the pre-commercialization period to 12% during the post-commercialization period. There were no differences in cannabis-related disorder rates between pre- and post-commercialization for young adults aged 18-25, adults aged 26-49, and older adults aged 50-70.

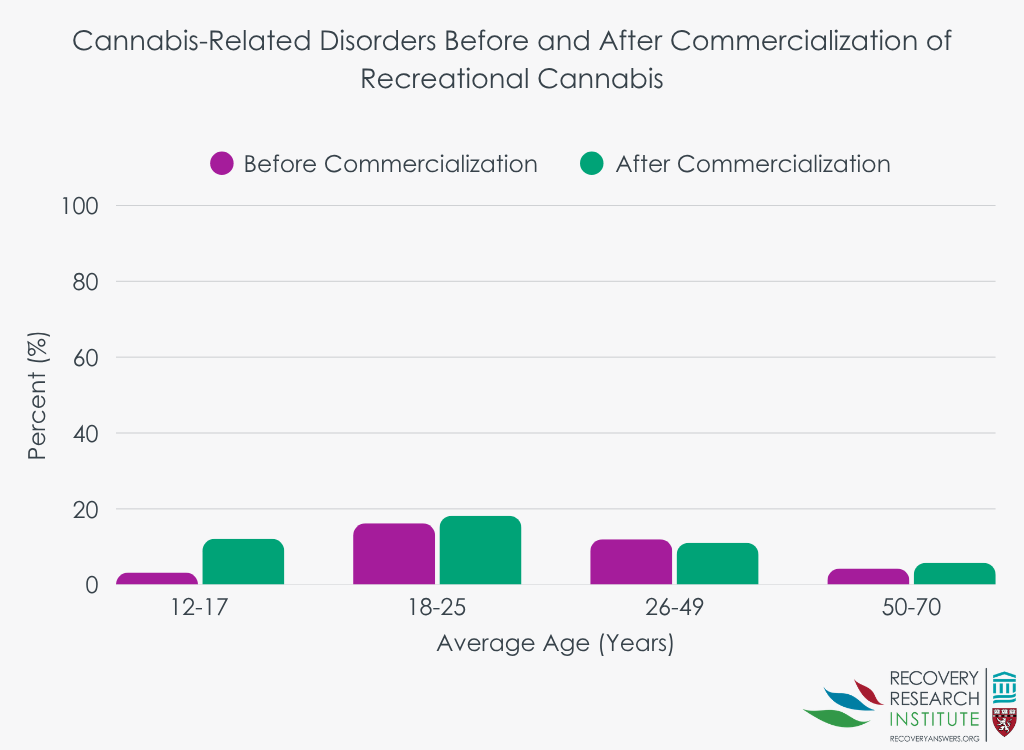
WHAT ARE THE IMPLICATIONS OF THE STUDY FINDINGS?
This study found that, among people with psychiatric disorders or vulnerabilities presenting to the psychiatric emergency room, legalization of recreational cannabis sales in MA was associated with increases in cannabis use, particularly for adolescents and adults aged 26-49. Results also showed that adolescents among this population were the only age group to have an increase in cannabis-related disorders. While there were only modest increases in rates of cannabis use among adults aged 26-49, and there were no increases in cannabis-related disorders for adults over the age of 18, the increases in both outcomes for adolescents are noteworthy. One important caveat is that emergency department doctors may be more likely to order urine toxicology screens or identify cannabis-related diagnoses among adolescents. This may reflect awareness of cannabis legalization as well as other potential risks, including the known epigenetic effects of cannabis and direct toxicity-related impacts on the adolescent brain. This could potentially increase the proportions in that age-group. Also of note, young adults 18-25 had the highest rates of cannabis use and cannabis-related disorder before and after legalization.
Even with the possibility of over-sensitization to adolescent cannabis use in mind, these findings among adolescents are particularly concerning given that early use of cannabis is associated with an increased risk of a variety of mental health conditions and cannabis use disorder is associated with suicidal behaviors among adolescents. Further, adolescence is an important stage of development, during which cannabis use can have especially harmful effects on the developing brain. Although expansion of legalization of recreational sales has not resulted in greater cannabis use for adolescents in the general population, it may be resulting in greater use among the most psychiatrically vulnerable adolescents. Expanded legalization may also result in ripple effects, such as research showing legalization of adult recreational cannabis use is associated with higher rates of overdose deaths among adolescents. Accordingly, although the study’s findings cannot be isolated to the effects of legalization of recreational sales alone, and causal effects cannot be demonstrated, findings underscore the need for prevention efforts to address cannabis among at-risk adolescents amidst changing policies.

BOTTOM LINE
Among people with psychiatric disorders or vulnerabilities, legalization of recreational cannabis sales was associated with increases in cannabis use, particularly among adolescents and adults aged 26-49, as well as an increase in cannabis-related disorders among adolescents. These findings underscore the need for specific cannabis prevention efforts among adolescents with, or at risk for, psychiatric disorders.
- For individuals and families seeking recovery: Increased access to cannabis in states with legalized recreational sales may unintentionally reach adolescents, particularly among those already experiencing or vulnerable to psychiatric symptoms. Families and young people may benefit from early conversations about cannabis risks and from seeking support early if mental health symptoms are experienced.
- For treatment professionals and treatment systems: These findings reinforce the importance of routinely screening for cannabis use among adolescents and adults with psychiatric conditions. Additionally, discussing potential risks associated with cannabis use, early education, and brief interventions in pediatric and behavioral health settings may help prevent cannabis use and cannabis-related problems among adolescents.
- For scientists: Because the study cannot demonstrate causal effects, future research that uses stronger causal designs would help clarify how legalization may cause increased cannabis use and cannabis-related disorders among adolescents. Also, because researchers could not separate the effects of legalizing medical marijuana from the effects of legalizing recreational sales analyzed in the current study, or from increased sensitivity to cannabis use and disorders among adolescents, future research would help disentangle these effects. Finally, because the study was conducted among patients in MA, additional research conducted in other states would shed light on the extent to which findings generalize to different state policy environments.
- For policy makers: As recreational cannabis sales continue to expand, these findings point to the importance of strong protections for adolescents alongside adult legalization policies. Continued investment in prevention, monitoring of youth cannabis trends, and policies that limit youth access may help mitigate unintended consequences for adolescents, particularly among those already facing psychiatric vulnerabilities.
CITATIONS
Foo, C. Y., Potter, K., Wright, A. C., Evins, A. E., Donovan, A. L., Levy, S., Mueser, K. T., & Cather, C. (2026). Effects of legalizing recreational cannabis sales on cannabis use and cannabis-related disorder among presentations to a psychiatric emergency service. American Journal of Preventive Medicine, 70(1). doi: 10.1016/j.amepre.2025.108142.

















